Oral cancer screenings at our office have been routine for the past 20 years, and I am continually amazed that new patients will come into our practice and ask, “What are you doing that for?” The “that” they are usually referring to is my palpating of the head/neck including the thyroid area looking for lumps and bumps that should not be there. Most of our patienst have nothing wrong in the mouth, head and neck area, but once in a while something shows up. One time it was a goiter on a woman who worked for an Ear, Nose and Throat doctor, and another time it was a swollen lymph node under the ear of a construction worker. In the latter case, I had mentioned to a patient that I felt a lump under his left ear and referred him to his physician for follow-up care. After a few weeks this very same patient came into the office without an appointment and wanted to speak with me in our private consultation room. When I met with him I could see out of the corner of my eye a long scar on his neck with staples still holding the incision together. He said, “I showed that lump to my primary care physician and he said it was probably nothing to worry about. But since you were concerned with it and told me to get it checked out, I went to an ENT on my own and he biopsied it. It was cancer and because of you, I have a chance to live.” Needless to say, we both cried, and this and other similar events has strengthened my resolve to examine each and everyone of my patients with extreme care looking for the tiniest chance that I may be saving their life.
Dentistry has found new links in the general health of patients over the past decades.
- The recent link between periodontal disease, cardiovascular disease, and strokes has affirmed the importance of dentistry as an essential medical provider.
- More people than ever are taking bisphosphonates such as Boniva and Fosamax to build up their bones to treat osteoporosis. This treatment has been reported in the literature to cause an increase risk of osteonecrosis (dying bone) in the maxilla and mandible. We have seen and have been referred a few cases from oncologists for this in the past few years.
- Head and neck radiation treatments for cancer destroys the tiny blood vessels in the jaws contributing to osteoradionecrosis (dying bone due to radiation).
- Radiation treatments can destroy the major salivary glands causing xerostomia (dry mouth), and xerostomia can cause radiation caries (cavities). The old treatment for this was fluoride trays, but now we are having good success with the Perio Protect Trays and Xylitol.
- Multiple common pharmaceuticals such as high blood pressure medications can cause xerostomia, drying up the mouth causing dentures to not fit, and dental cavities. Xylitol is helping with this problem quite a bit.
- Diabetes mellitus can cause dramatic infections in the mouth that will compromise routine treatments such as scaling and root planing and implant placement. Monitoring the patients HgA1c levels is an important means knowing if the blood sugar has been stable over the past 3 months.
- Esophageal reflux and GERD (gastroesophageal reflux disease) can cause acid erosion of the teeth contributing to cavities, loss of enamel, and tooth sensitivity.
- Bulimia– can have the same effects as GERD
- Sjogren’s Disease– an autoimmune disease that attacks the exocrine gland such as the salivary and tear gland causing xerostomia (dry mouth).
- Scleroderma– a connective tissue disease causing the skin of the face to tighten so much it may be hard to open the mouth wide enough to work inside.
- Systemic diseases can cause dramatic weight loss/gain thus shrinking/expanding the oral tissues making denture loose/tight.
- Cancers that start in other parts of the body can show up in the mouth with signs of metastasis and visa versa.
- Obstructive Sleep Apnea is being treated with non-traditional oral appliance therapy. Many people being diagnosed with OSA and prescribed CPAP, but cannot tolerate the hose in their nose. OSA is linked to diabetes, high blood pressure, high cholesterol, daytime sleepiness, and adult ADHD.
Medical Health History
Every dental office in the modern world requires their patients to fill out a medical history of some kind. The form is usually designed to be as simple and as quick to fill out as possible. Yet, no matter how simple we try to make it to fill out, there are still patients who ignore it by drawing lines through entire blocks of questions/diseases/symptoms and omitting pertinent information just to save a few minutes of “grief”. Then they sign the “legal document” not realizing that this is the standard the doctor will be held to when treating them.
The importance of filling out the medical health history properly cannot be overstated. Take your time and think about every question before filling them out completely. It is essential in giving the doctor the right information to treat their dental problems.
Oral Cancer Screening
Face:
- Symmetry: Although the face is generally not exactly symmetrical, you can tell that something is wrong if one side is grossly different from the other. The eyes should be roughly the same size and level with the ground, the cheeks the same height and size, the nose should appear normal (huge variations), and the lower jaw should be the same from one side to another.
- The facial forehead, mid-face and mouth regions should be roughly cut into equal thirds.
- Color: localized redness (heat?), brown or black pigmented lesions, telangiectasia, lesions, scars.
- Drooping: Eyes, cheeks, lips either bilaterally or unilaterally.
Lips:
- Symmetrical
- A well defined border between the lips and facial skin (vermillion border). This area is a high risk area for squamous cell carcinoma. Basal cell carcinoma can also be found in this area.
- Smooth, non-scabby texture
- No light or dark spots- hemangioma, mucocele, herpes
- No ulcerations- Herpes Simplex, solar cheilitis, trauma, squamous cell carcinoma, sun burn, seborrheic keratosis
- Scars- past history of surgery, trauma
- Lumps or bumps-palpation of the lips can reveal abnormalities within the lips themselves that cannot be seen with the naked eye.
Oral cavity:
Basically, dentists are specialty physicians of the stomatognathic system (mouth). Although we take many of the initial courses that medical doctors take in school, we quickly divert into our own specialty in which few medical doctor understand. Dentists look for red (erythroplakia), white (leukoplakia) lesions, at the palpate for indurated (lumps) and fixated masses (bumps) inside the tissues of the head and neck
- Inner lining of the lips is called the vestibule- This is were chewing tabacco is placed.
- The gums around the teeth are called the gingiva- this is keritinized attached tissue that is usually hard enough to resist the scrapping trauma of crunchy foods. It can be broken down by gum disease and develop pathology such as pyogenic granulomas.
- Floor of the mouth- this is a high risk area. The submandibular salivary glands are located on other side of the frenum under the tongue. Any masses that feels firm or fixated in position are of high risk for cancer.
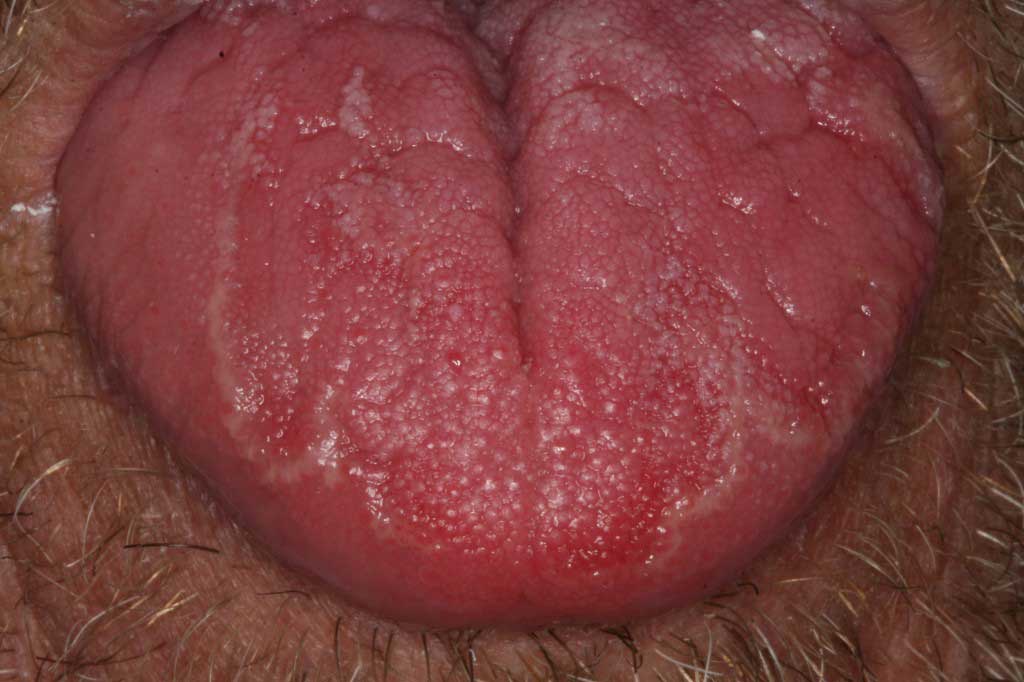
- Tongue- the top is at less of a risk than the sides of the tongue (lateral borders). The base of the tongue buried deep inside the tissue is of high concern as well. It should move without spasms or asymmetry (hypoglossal nerve damage). Circumvallate papillae and lingual tonsils are normally found on the top and sides of the tongue, and are often mistaken for pathologic lesions. Cracks and fissures can be a normal variation of the tongue anatomy. A tongue with “bald” stops or a brown color could indicate a yeast infection. Yeast infections could mean an immunity problem (blood borne cancer, HIV/AIDS).
- Hard and soft palate- The soft palate is more often seen as a place for pathosis than the hard palate. Red spots, white spots, ulcerations, rough areas, asymmetry, growths, or other masses may be the first sign of a cancer. If the uvula doesn’t hang down in the midline of the soft palate, a mass may be pushing it to one side or vagal nerve palsy. A very hard lump in the midline of the hard palate may be a torus palatinus which is a normal variation of anatomy (a normal abnormality).
- Tonsillar, adenoids, nasopharnyx- These areas can be hard to see without a special scope (ENT). We usually use a 2X2 inch gauze to pull out the tongue and a mouth mirror to look down the throat. Watch it! Looking too deep may gag and cause reverse peristalsis!
- Retromolar pad- This is the area just past the last lower molars
- Tuberosity area- This is the area just past the last upper molars.
- Buccal mucosa- This is the inner cheek area. Some people have the habit of chewing their cheek and this results in a white line on the cheek called the linear alba (normal and does not cause cancer). Chewing tobacco can irritate this area of the mouth. Diseases like lichen planus can be easily seen on the cheeks (Wickman’s striae).
- Parotid/Stensen’s duct- This duct is found in the upper part of the buccal mucosa at the level of the maxillary 1st and 2nd molars. It is the opening to the major salivary gland, the parotid. It can be “milked” by the doctor to see if it is flowing properly. The fluid come out of this duct should be clear, thin and of high volume. Milky looking fluid means an infection. Infection are usually cause by the saliva becoming stagnate inside the gland by some kind of blockage.
- The parotids are the largest salivary glands and are situated in the cheek areas in front of the ears. Various pathologies/blockages including stones, viral infections, bacterial infection, benign and cancerous tumors can occur in this region.
Neck:
The neck should look symmetrical. Checking the neck for lumps and bumps that should not be there is very important to detecting oral cancer. It is believed that a swollen lymph node in this area that is hard and fixed and not painful is most likely metastatic cancer. A primary cancer in the oral cavity would need to be ruled out.
Lymph nodes chains to palpate:
- Jugular chain first: Along the side of the neck following the sternomastoid muscles from the ear to the clavicle.
- Parotid gland: In front of each ears.
- Submental: Under the chin
- Submaxillary chain. Under the lower jaw
Thyroid:
The normal thyroid gland is actually hard to palpate. It is only when a lump or bump or the gland is swollen that anything is noticeable. If tenderness, hardness or a cystic feeling is found in this area, you should seek medical consultation.
Risk Factors for Oral Cancer:
- Smoking: Researchers have discovered cigarette smoke slows the production of a protein called FANCD2. FANCD2 is a ‘caretaker’ proteins for DNA damage in the cells. If you do not make enough FANCD2 to fix the damaged DNA inside cells, it can causes the faulty cells to go hay-wire (cancer).
- Alcohol: Alcohol is an irritant in the mouth and throat. It damages the cells and when they try to repair themselves, it may lead to DNA changes in the cells which can be a step toward cancer.
- Sun: Prolonged exposure to the sun can cause pre-cancerous (actinic keratosis) and cancerous (basal cell carcinoma, squamous cell carcinoma and melanoma) skin lesions. The radiation from the sun can cause the loss of the skin’s immune function; fine and coarse wrinkles; freckles; mottled pigmentation; sallowness (yellow discoloration of the skin), telangiectasias (the dilation of small blood vessels under the skin), and elastosis (the destruction of the elastic tissue causing lines). I other words, the sun eventually makes your skin look, feel and act OLD.
- History of past cancer: Having a past history of cancer means you once had the right conditions to have cancer, and those same conditions may pop up again.
- Human Papalloma Virus (HPV):
Free Head and Neck Oral Cancer Screening:
Our office has joined the Head and Neck Cancer Alliance (formerly known as the Yul Brynner Head and Neck Cancer Foundation).
We offer free Head and Neck Oral Cancer screening by appointment at our office during regular working hours. A SCREENING consists of a visual and physical examination of the head and neck. It does NOT included a dental exam (for tooth decay/periodontal disease), cleaning, restorations, or any x-rays. It is only a free screening.
THE PATIENT AND ANY OTHER PERSON RESPONSIBLE FOR PAYMENT HAS A RIGHT TO REFUSE TO PAY, CANCEL PAYMENT, OR BE REIMBURSED FOR ANY OTHER SERVICE, EXAMINATION, OR TREATMENT THAT IS PERFORMED AS A RESULT OF AND WITHIN 72 HOURS OF RESPONDING TO THE ADVERTISEMENT FOR THE FREE, DISCOUNTED FEE, OR REDUCED FEE SERVICE, EXAMINATION, OR TREATMENT. Expiration date 12/31/12
Typical Benign Lesions:
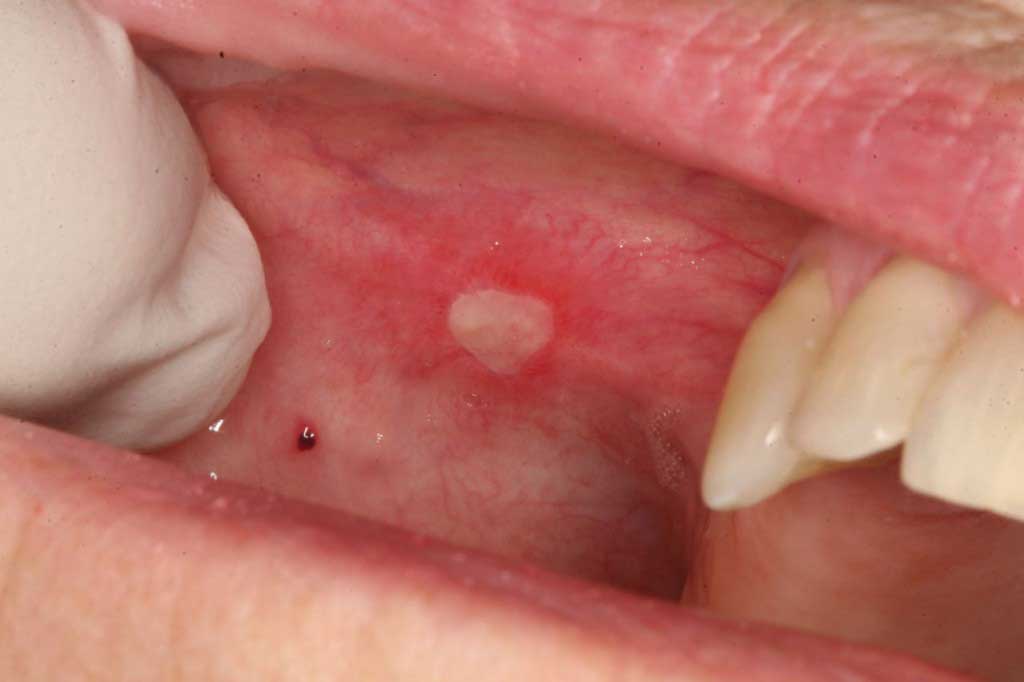
- Aphthous ulcers: These lesion are so common and obvious, they can be diagnosed over the phone. They are usually roundish in shape, have a white center and a red border. When you put your tongue on it it usually burns or STINGS! Many people get them after eating something acidic, like orange juice, tomato sauce, or pickles. There are various remedies, but the one we use with great success is a prescription mouthwash called Peridex. If you are a doctor and are reading this for the first time you are rolling your eyes about now, and saying this guy is dead wrong. True, Peridex will not work on an aphthous ulcer as a mouthwash, BUT if you completely soak a cotton roll in it, and place it over the lesion for at least 15 minutes (and I mean 15 minutes), the lesion will go away quickly. Other ways include laser cauterization. They are self limiting and usually go away over the period of a week or two without any treatment. Occasionally, a major aphthous ulcer will form and be so painful the patient cannot swallow food with extreme discomfort. The laser is the best cure for this type of lesion, but Peridex/cotton ball works satisfactorily as well over time. HOWEVER, aphthous ulcers may just be the tip of the iceberg and can be an indication of a more serious health condition, such as an autoimmune disorder, human immunodeficiency virus, Crohns Disease, and hematologic or oncologic conditions
- Pyogenic granuloma: Also known as a pregnancy tumor because it common forms on the gum lines of pregnant women. They are red growths that usually show up between the teeth where a recent trauma has occurred (flossing trauma, food impaction, carious lesion). They can also form on the skin. We remove then with a laser.
- Peripheral Giant Cell Granuloma: Looks like a pyogenic granuloma and can only be differentiated by histology. It is more aggressive and can “cup-out” out bone around it. Once it is identified by a biopsy it it removed with a laser. It can reoccur.
- Herpes simplex: I used to say if we treat it it will go away in 14 days, and if we do not treat it it will go away in 2 weeks, because there weren’t any very good ways to treat herpes simplex type 1… until NOW!
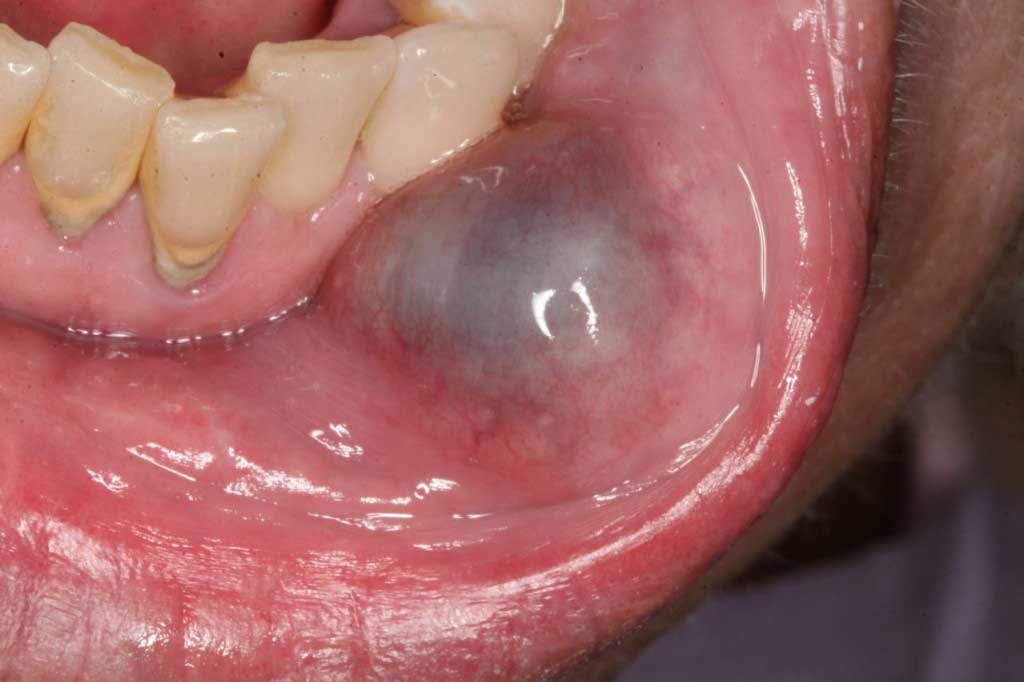
- Ranula: This is a traumatized salivary gland that has blown up as big as a “frog’s belly”. It is named after a frog’s belly (Rana is a genus of frogs). When a salivary gland functions properly it makes a lot of product. This product (saliva) flows through a small opening out into the mouth to moisten the mouth. When this small opening becomes damaged it can scar over blocking the saliva’s way out. This can cause the tissue around the salivary gland to blow up like a big bubble that must have looked like to someone a frogs belly. The treatment is simply to pop the balloon, we do it with a laser. The only problem is that they can reoccur.
- Fibroma: Everyone has bit their cheek, tongue or lip at one time in their life. This trauma usually heals without any trouble. However, once in a while the area will scar to a point that it becomes an area of the mouth that you bite more often than others. This scarring can become a large tissue tag that becomes a nuisance and can show when you talk. Removing it with a laser in a simple procedure.
- Benign Migratory Mucositis: Also known as Geographic Tongue because it looks like the outline of a land mass on a map on your tongue/cheeks. It is a lesion of unknown etiology that actually moves around the mouth over time.
- Lichen Planus: Dentist will say that this is typically a condition of the mouth that sometimes expresses itself on the wrists and ankles; but the dermatologists will say it is primarily a condition of the wrists and ankles that occasionally will show up in the mouth. In the mouth, the most common reticular form shows up as white linear streaks called Wickman’s Striae and usually goes unnoticed by the patient. The bullous form has fluid-filled vesicles that can break and cause some irritation. The erosive forms is erythematous (red), ulcerated and uncomfortable. This form has been thought to have a less than 1-5% malignant transformation, although this conclusion is controversial. The treatment is usually steroids.
- Parulus: This usually shows up as a whitish/yellow pimple over the neck of a tooth. It is the opening to a draining abscess. The doctor will need to find and treat the dead tooth responsible for the draining infection and either treat it with a root canal or extraction. As long as the parulus stays open and drains properly the tooth may feel comfortable and not swell. However, at anytime the opening may close and the subsequent back pressure of puss will cause a swelling and toothache. Best to seek definitive treatment before this happens!
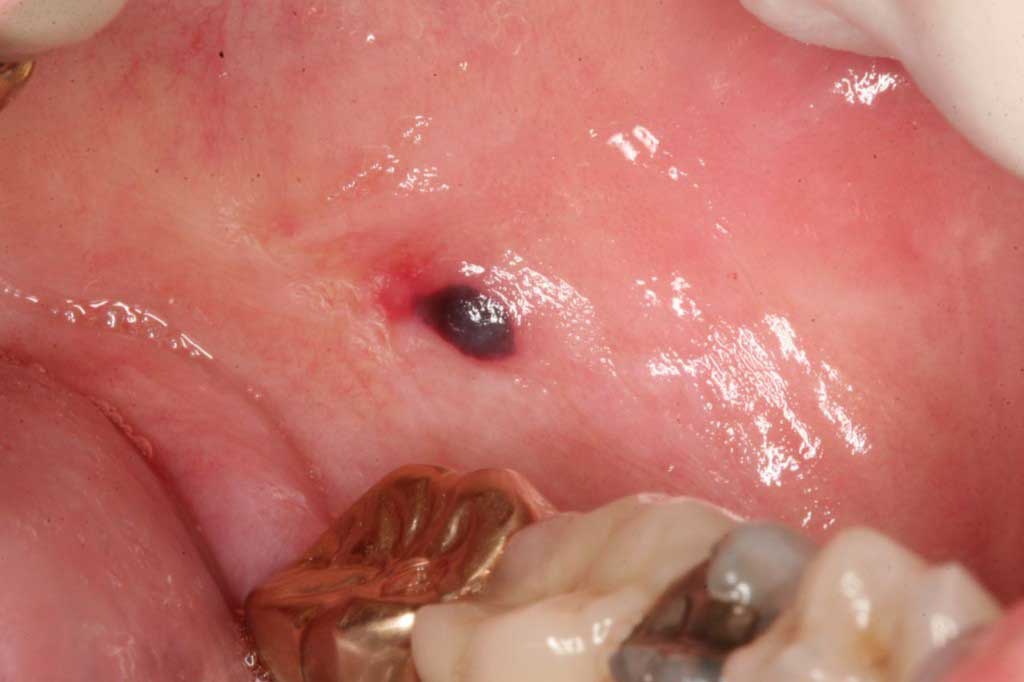
- Mucocele: This is simply a backed up minor salivary gland. They can appear anywhere in the mouth or lips as a black translucent spot that does not blanch when depressed. We treat these with a laser. They may reoccur over time.
- Hemangioma: They appear the same as a mucocele, but do blanch when depressed. This means they are made of a glob of blood vessels bunched up together to make the spot look dark. They can be very difficult to remove surgically because of the bleeding from blood vessels, but are exceedingly simple to remove with a laser.
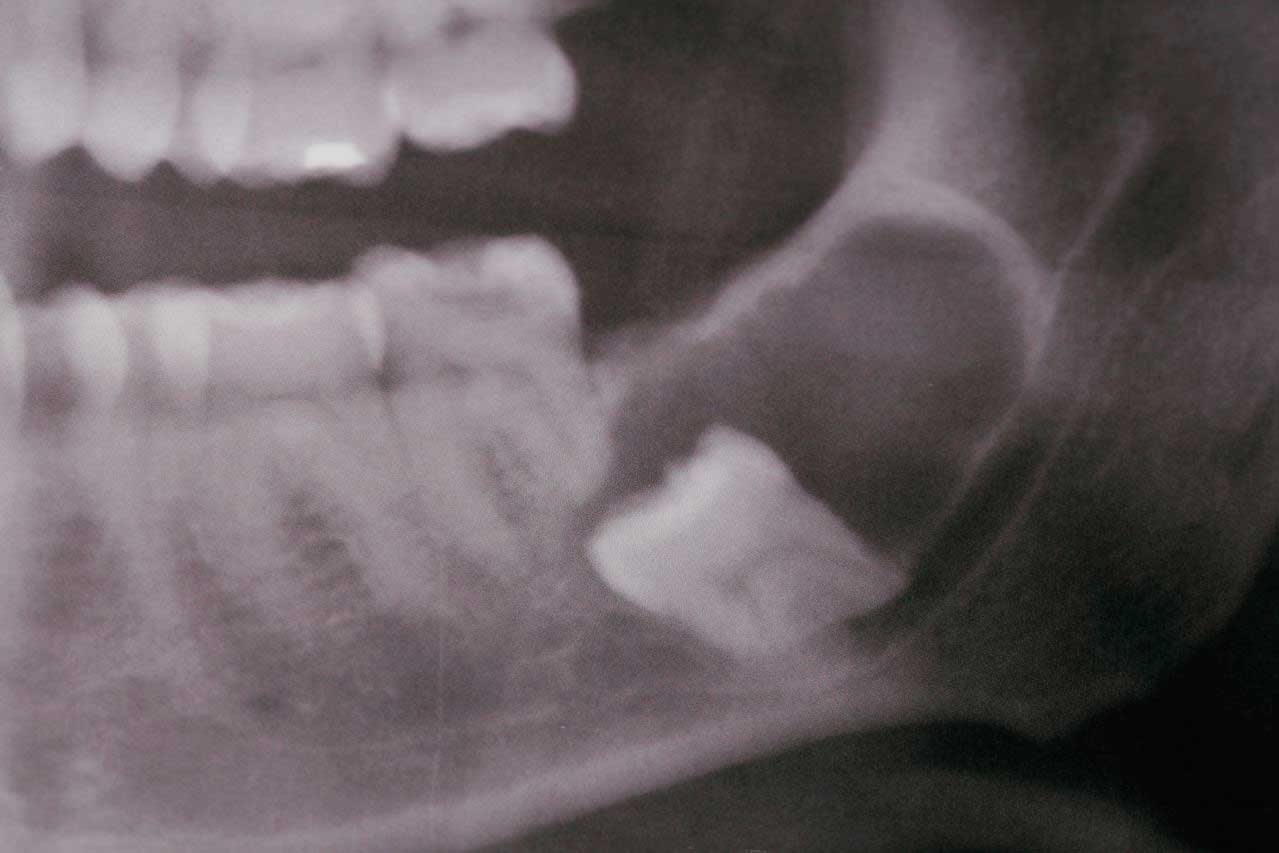 Radiographs:
Radiographs:
Dental radiographs cannot tell if you have cancer, they can just show the doctor where something abnormal is located. Certain patterns in the bone may suggest cancer, but only a biopsy of the area can differentiate cancer from other boney lesions.
Lesion Photographs:
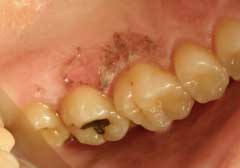
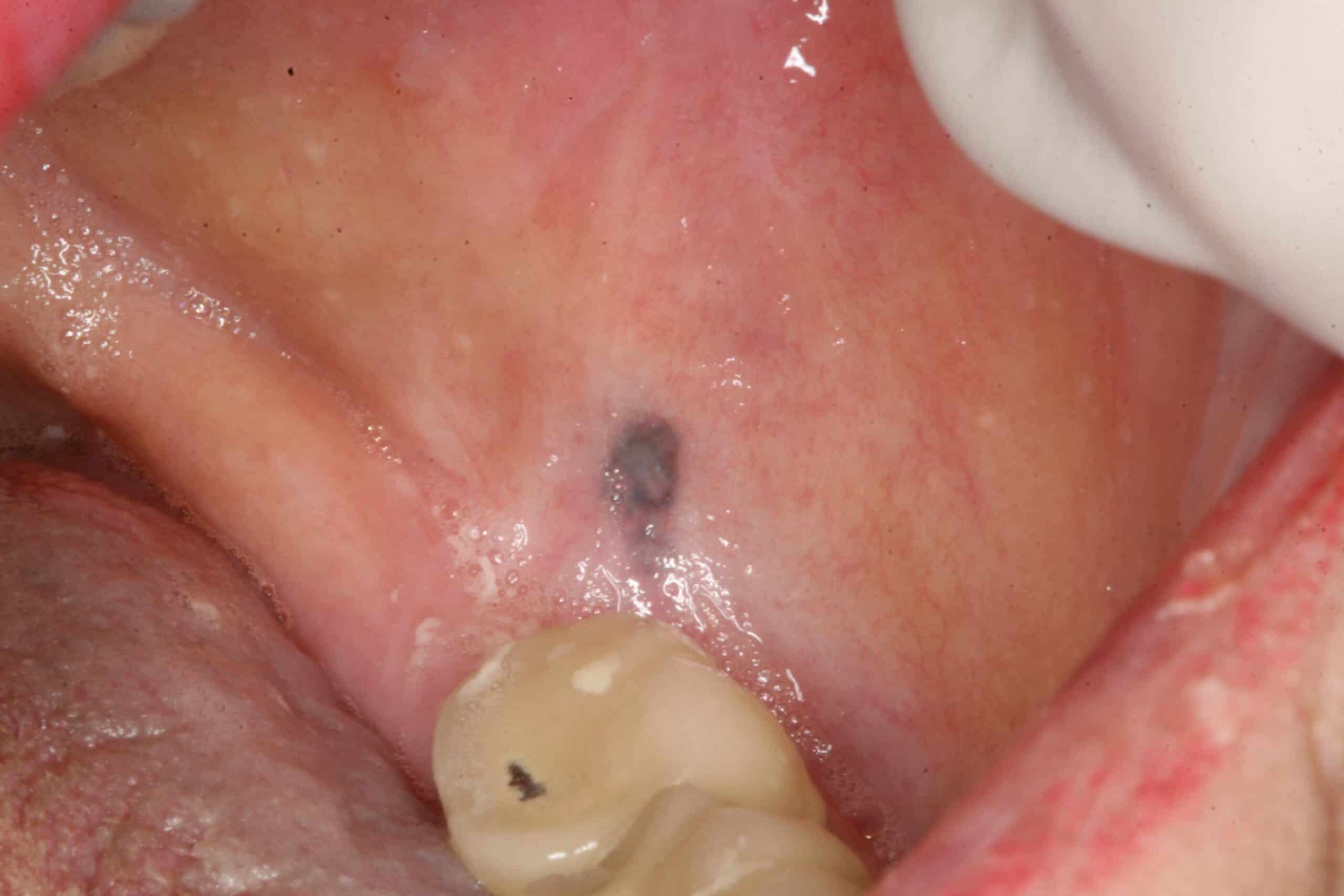 Amalgam tattoo: Lower 3rd molar region. Benign. This can happen when a piece of a silver filling is left in the extraction site to “rust” and cause what looks like a tattoo. This lesion can be confused with malignant melanoma.
Amalgam tattoo: Lower 3rd molar region. Benign. This can happen when a piece of a silver filling is left in the extraction site to “rust” and cause what looks like a tattoo. This lesion can be confused with malignant melanoma.
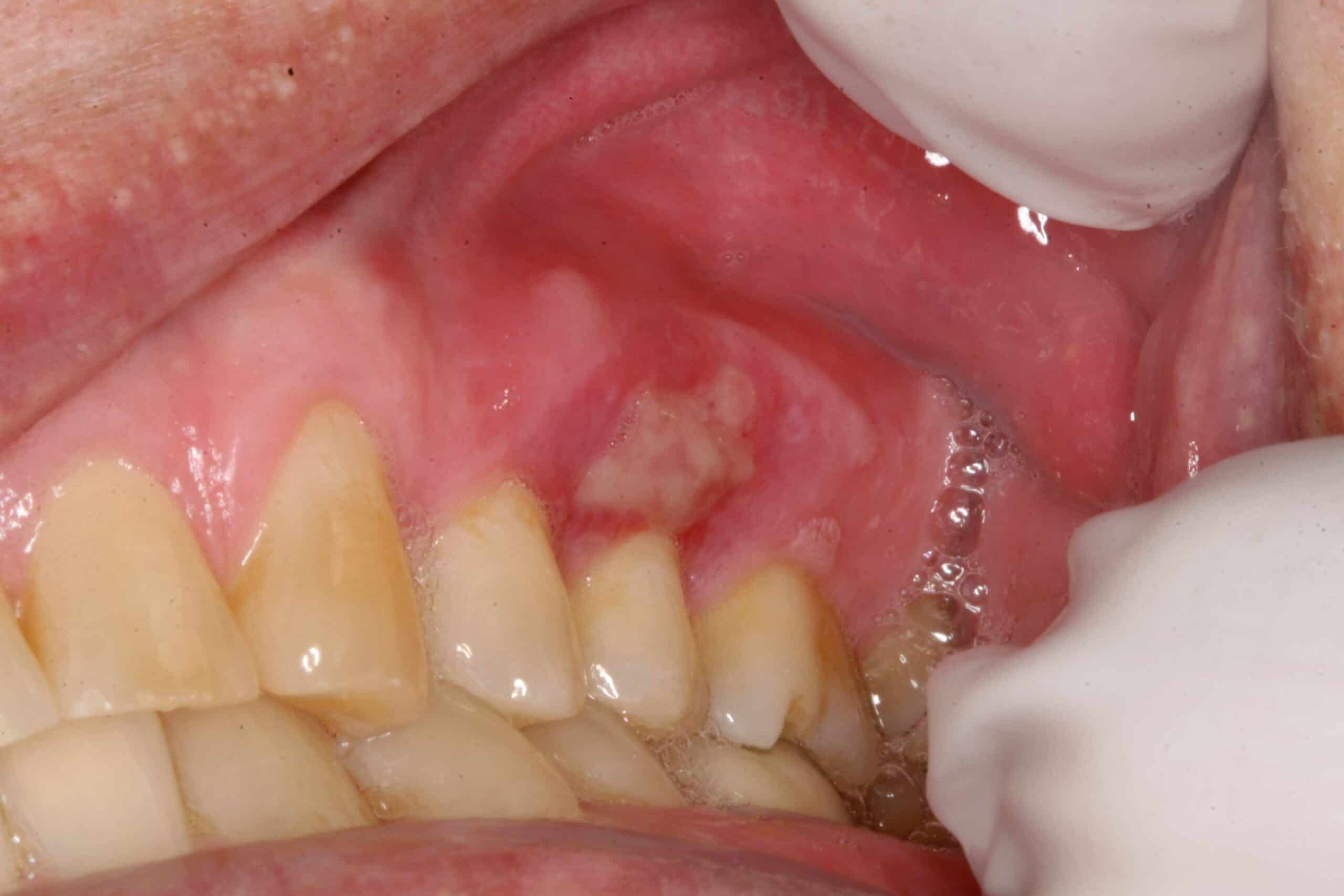 Toothbrush trauma: Benign. This usually happens right before a dental exam and cleaning. I guess they feel if they scrub really hard it will undo all the neglect they gave their teeth between check-ups.
Toothbrush trauma: Benign. This usually happens right before a dental exam and cleaning. I guess they feel if they scrub really hard it will undo all the neglect they gave their teeth between check-ups.
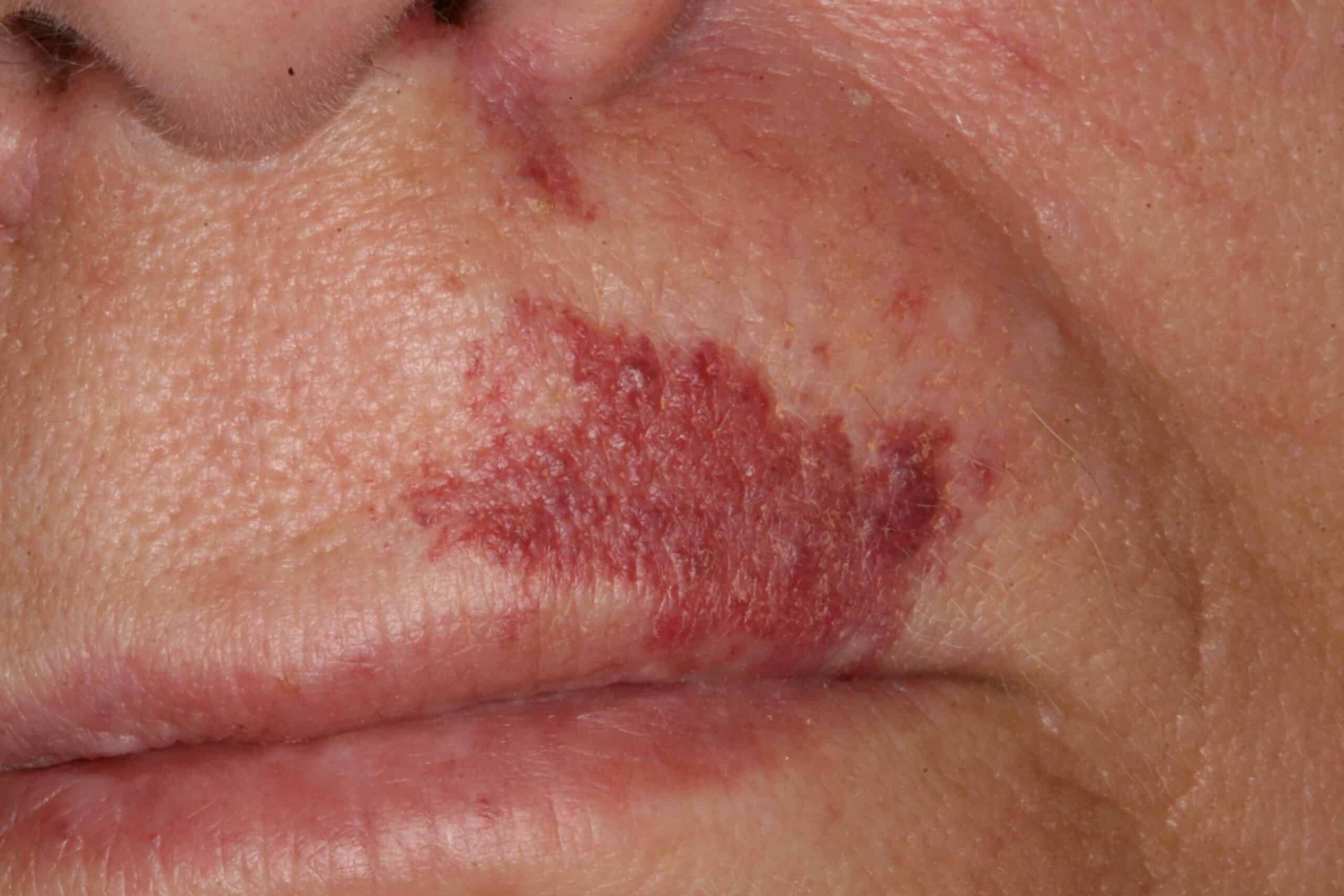 Port Wine Stain: Benign. A birth defect of blood vessels.
Port Wine Stain: Benign. A birth defect of blood vessels.
 Trauma: Benign. This looks very bad but usually heals very well.
Trauma: Benign. This looks very bad but usually heals very well.
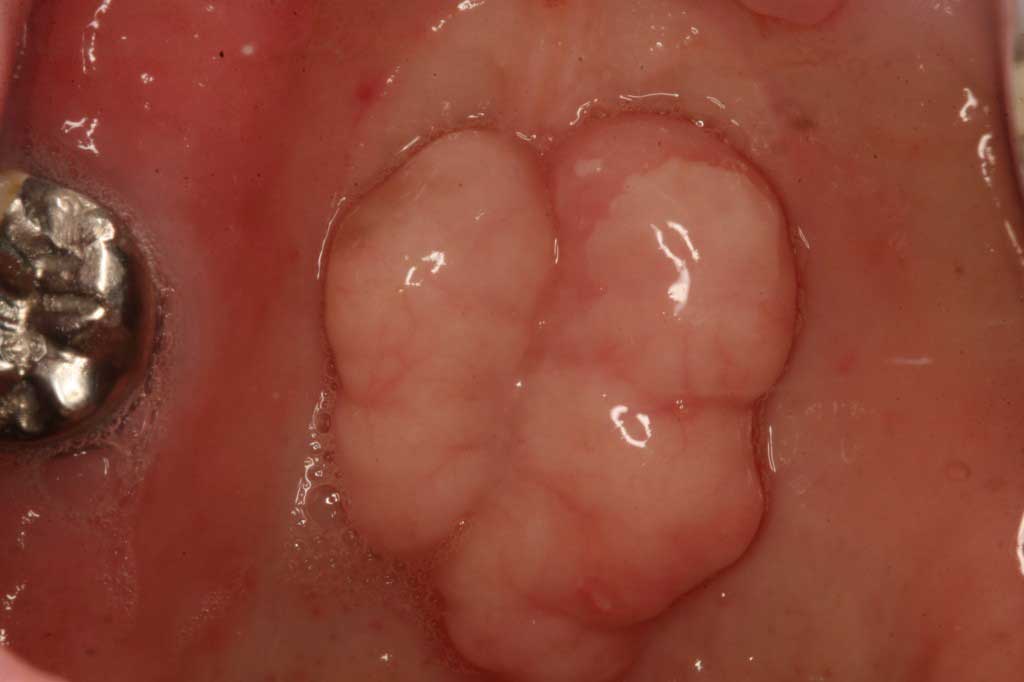
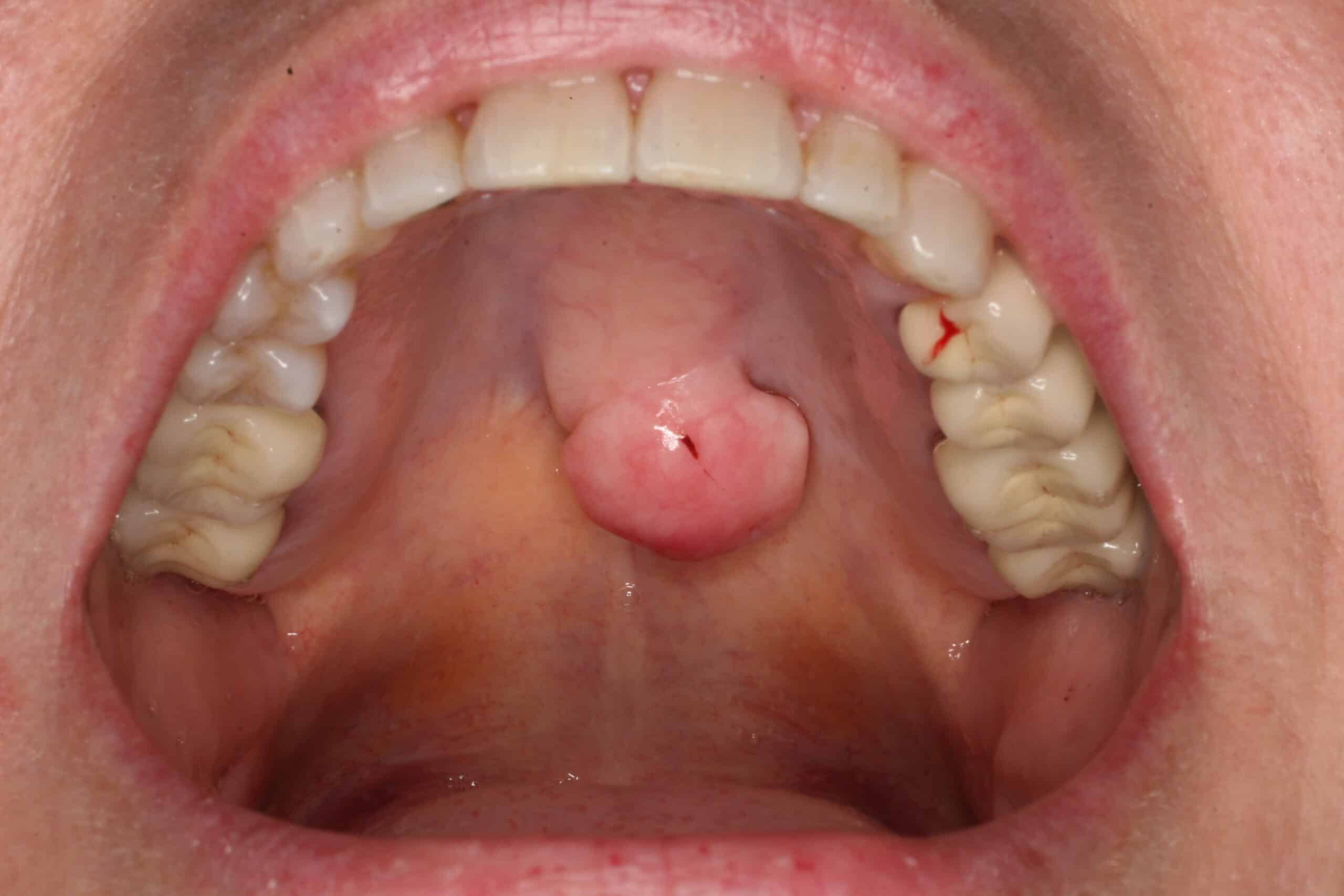
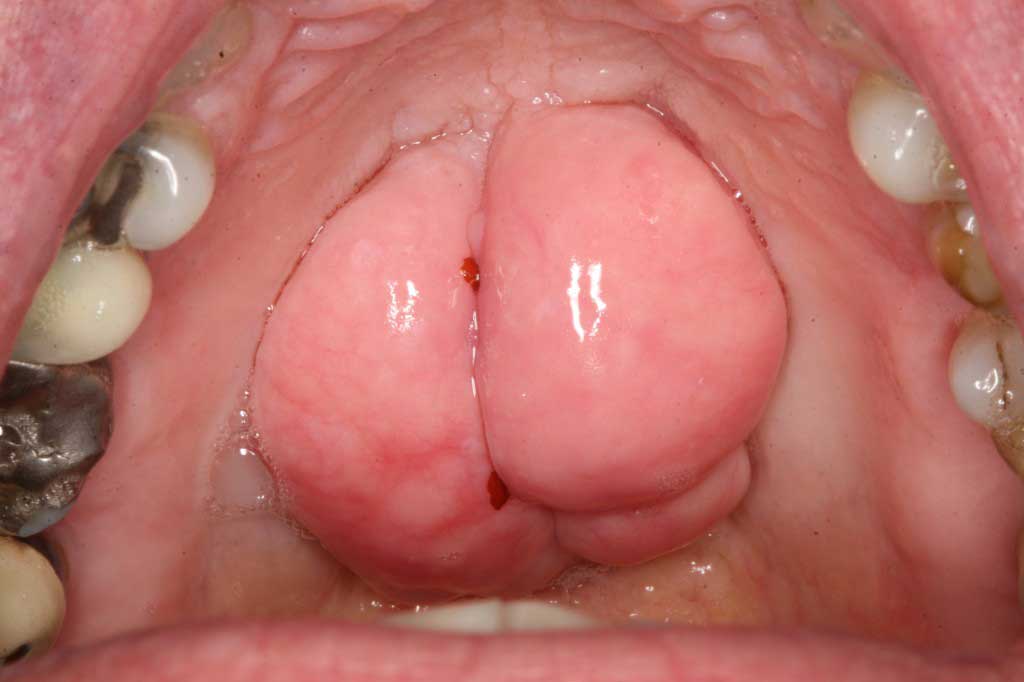
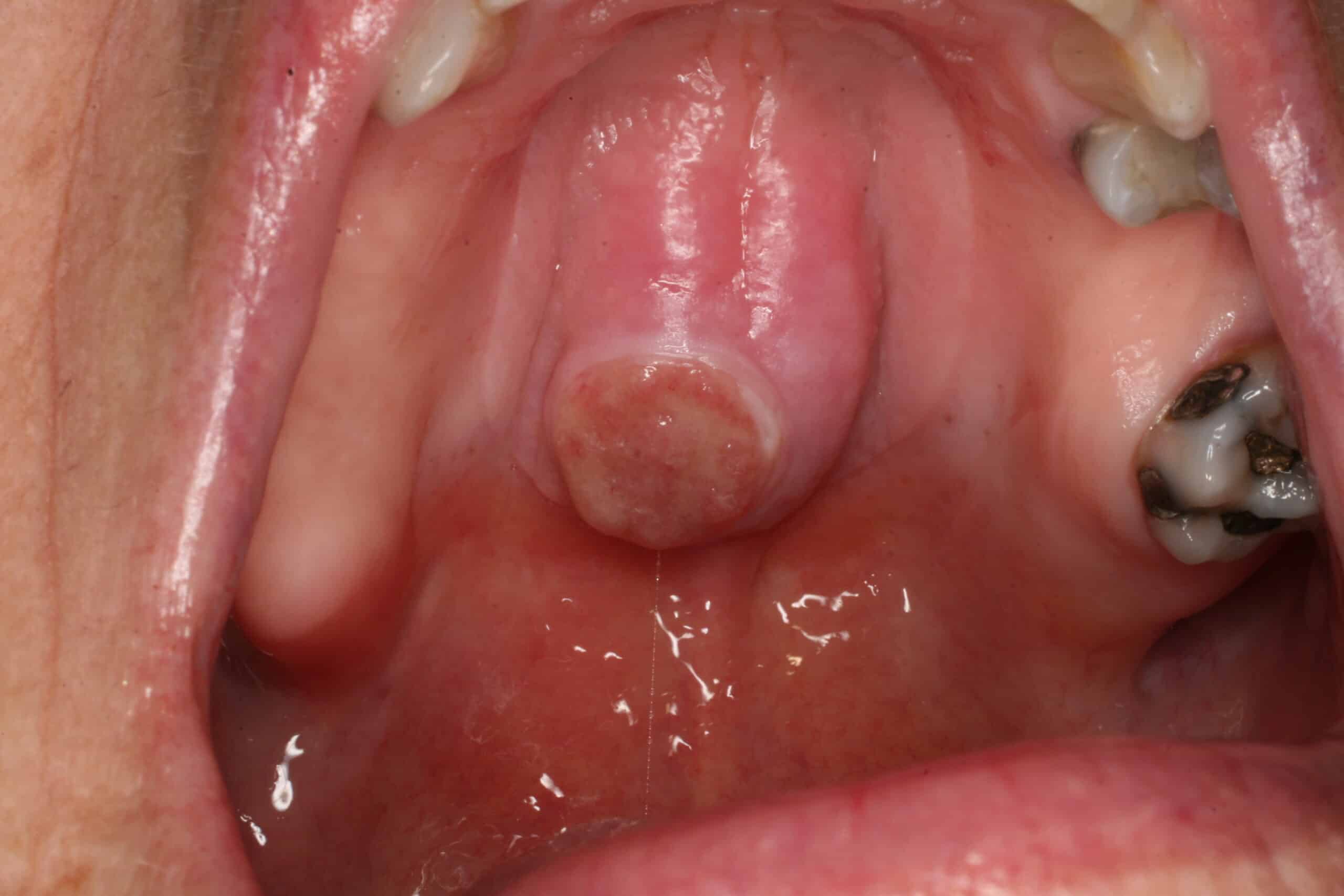 Tori Palatini: Benign. This is a common and completely normal boney growth in the middle of the palate. It comes in many sizes and forms. People who have these do not know that other people do not have these in their palates. In the last photo the tori had been traumatized by food or other trauma and completely healed after one month. My instructor in dental school called these boney growths, “Normal abnormalities”.
Tori Palatini: Benign. This is a common and completely normal boney growth in the middle of the palate. It comes in many sizes and forms. People who have these do not know that other people do not have these in their palates. In the last photo the tori had been traumatized by food or other trauma and completely healed after one month. My instructor in dental school called these boney growths, “Normal abnormalities”.
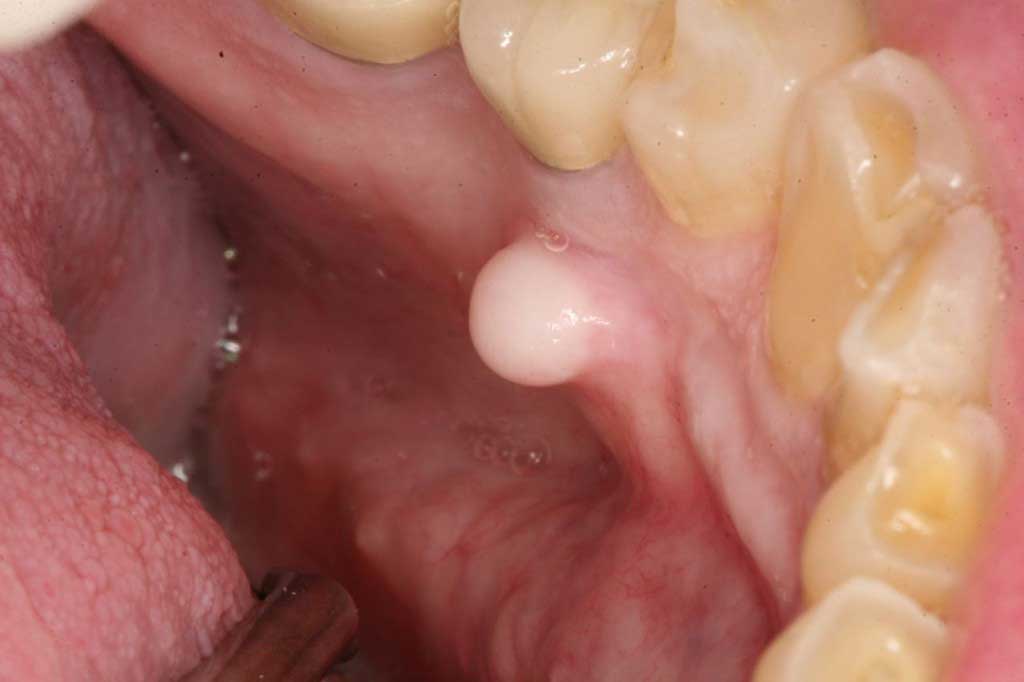
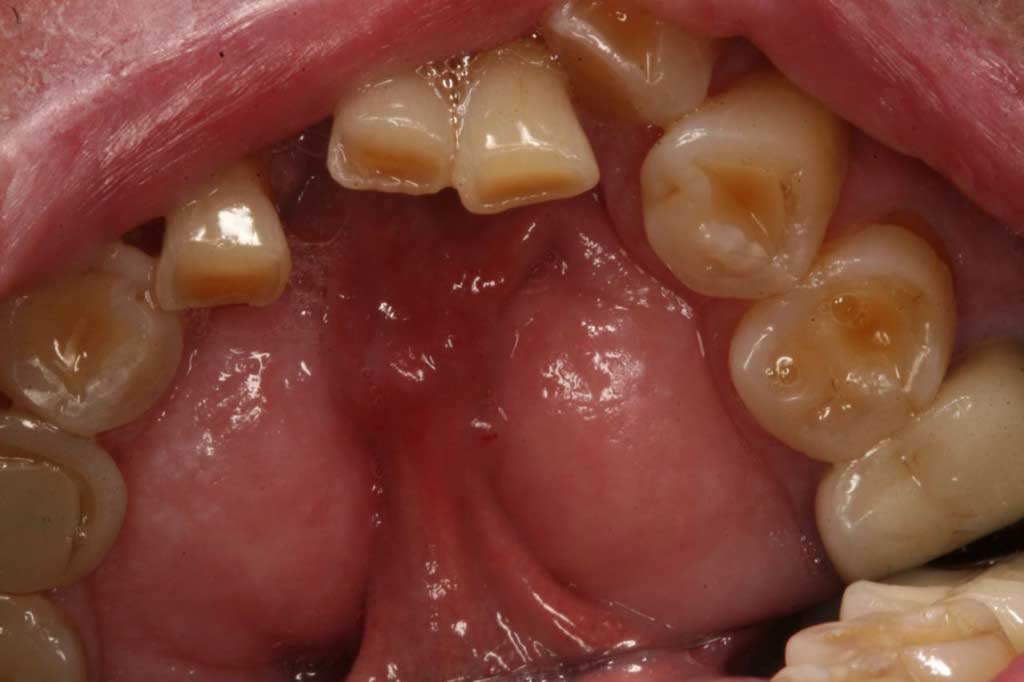
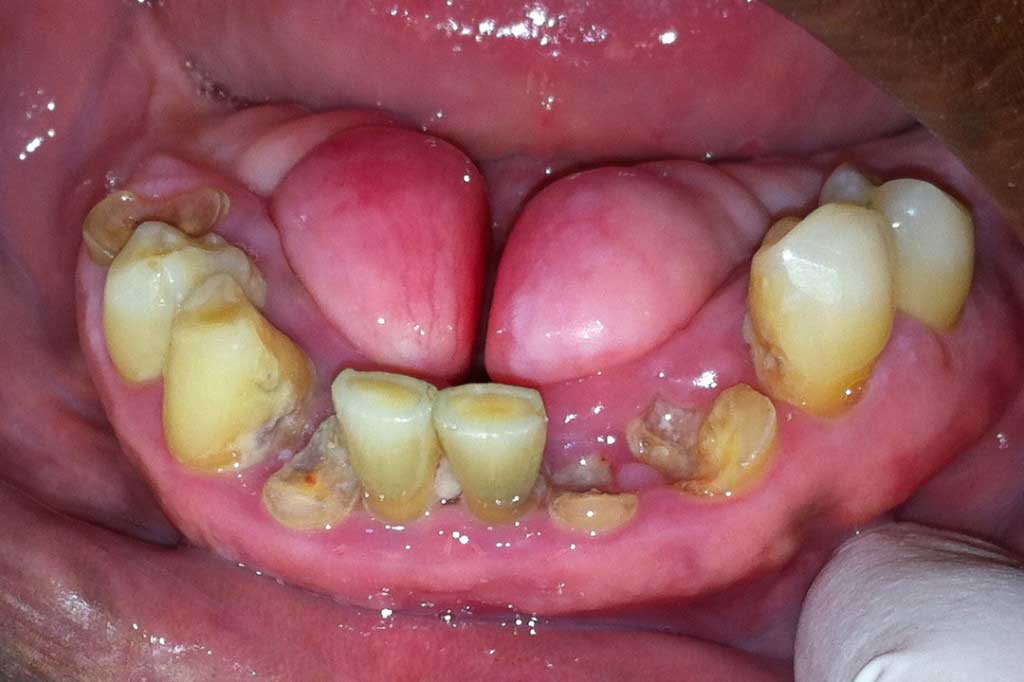 Mandibular Tori: Benign. Some mandibular tori are very small and some can be so large they can crowd out the tongue space.
Mandibular Tori: Benign. Some mandibular tori are very small and some can be so large they can crowd out the tongue space.
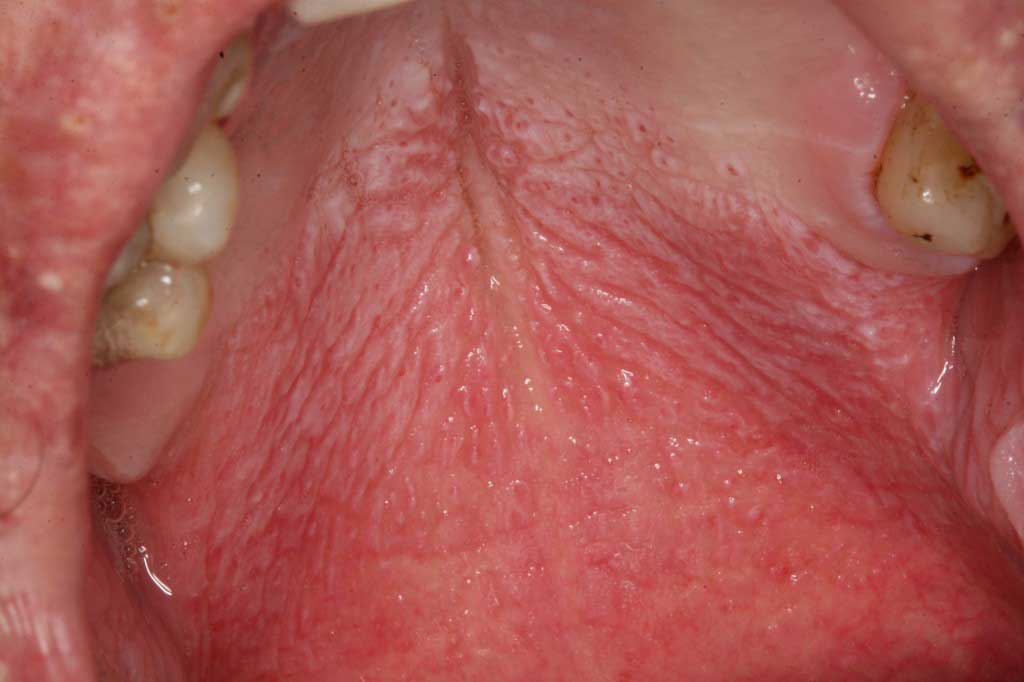 Nicotine Stomatitis: Pre-cancerous. This is on the palate and occurs on the cheeks and gums as well. The combination of the cigarette/cigar/pipe smoke and heat causes the tissue to swell and turn white (thicken) with red irritated spots and streaks.
Nicotine Stomatitis: Pre-cancerous. This is on the palate and occurs on the cheeks and gums as well. The combination of the cigarette/cigar/pipe smoke and heat causes the tissue to swell and turn white (thicken) with red irritated spots and streaks.
Palatal cancer. Squamous Cell Carcinoma. Rare. Found under an ill-fitting denture. Differential Diagnosis was necrotizing sialometaplasia, Gumma, minor salivary gland tumor, midline lethal carcinoma (usually seen in children). It was diagnosed by biopsy and sent to an oncologist for treatment. This was treated with radiation and has not reoccured.
Pizza burn: Upper back palate. Benign. Any hot food can burn the mouth.
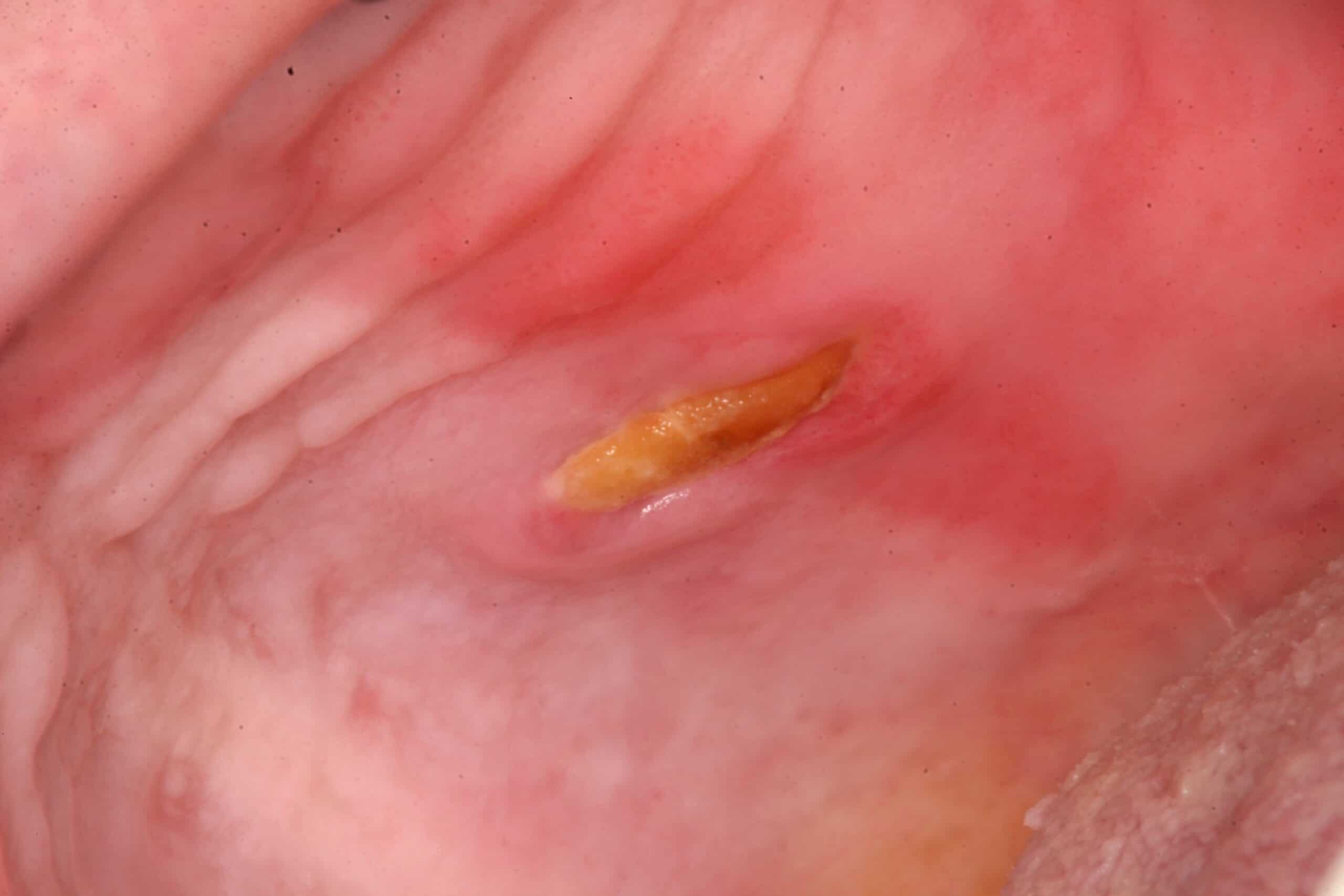
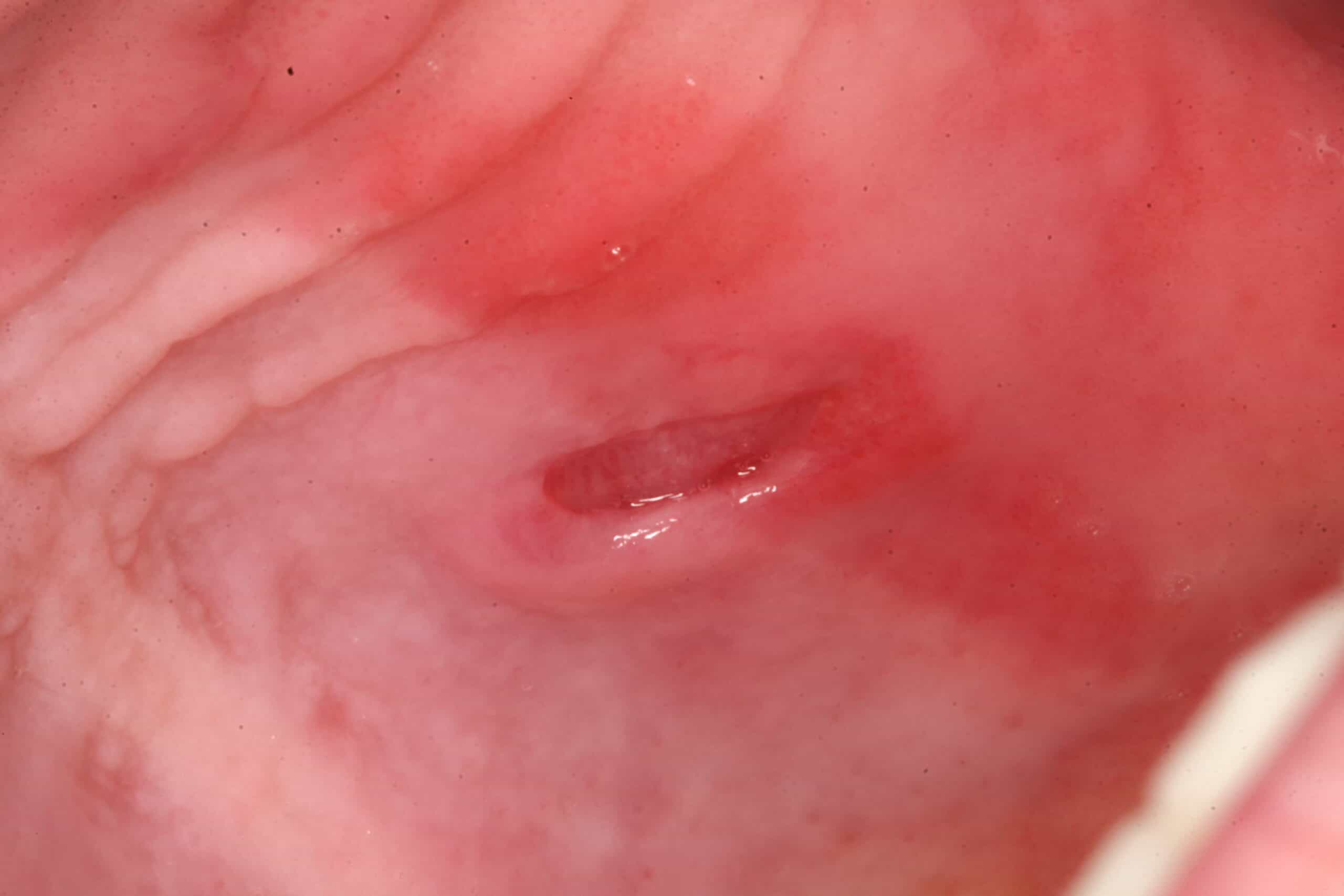 Food Trauma: Palate. Benign. This is a before/after picture of a popcorn hull stuck to the palate under a denture long enough to have tissue grow around it.
Food Trauma: Palate. Benign. This is a before/after picture of a popcorn hull stuck to the palate under a denture long enough to have tissue grow around it.
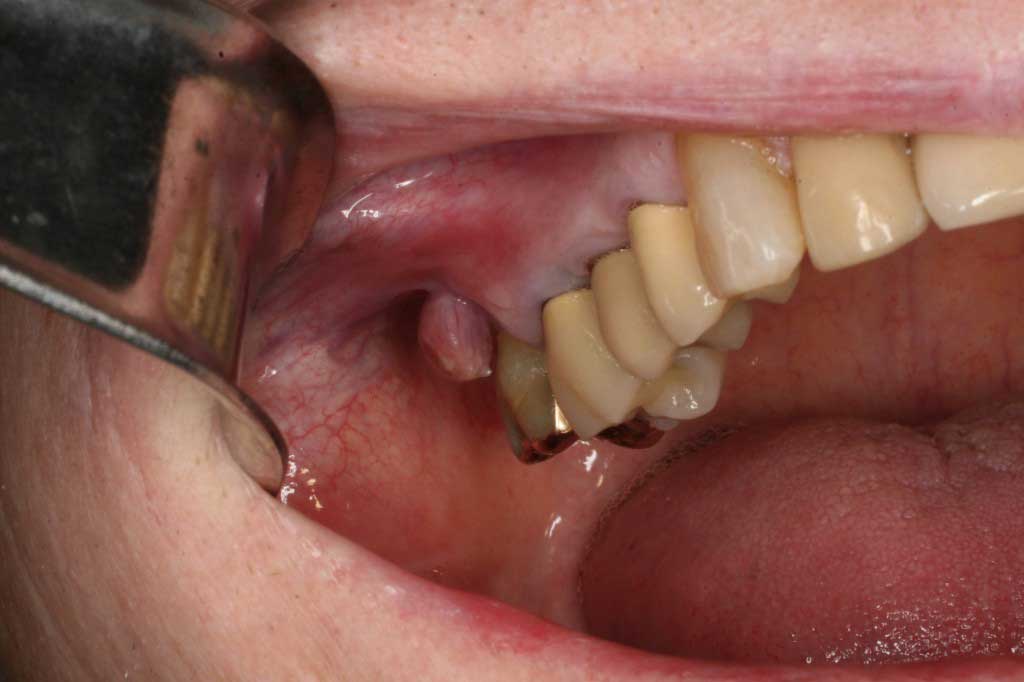 Parulus: Benign. Bacterial infection. This is a draining abscess from the last molar (second molar)
Parulus: Benign. Bacterial infection. This is a draining abscess from the last molar (second molar)
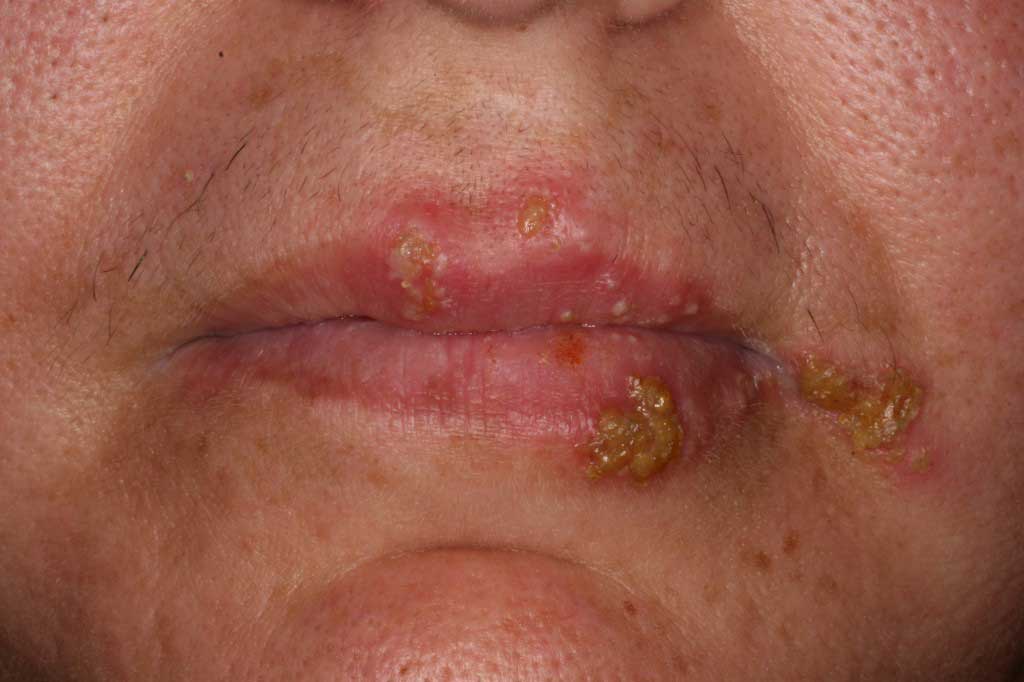 Herpes Simplex 1: Benign. Viral infection. A very bad case of herpes (common cold sore). It is unusual that the lesion has spread across the midline of the mouth. (Assumed to be HS1, but could be genital herpes). Laser treatment or chemical treatment
Herpes Simplex 1: Benign. Viral infection. A very bad case of herpes (common cold sore). It is unusual that the lesion has spread across the midline of the mouth. (Assumed to be HS1, but could be genital herpes). Laser treatment or chemical treatment
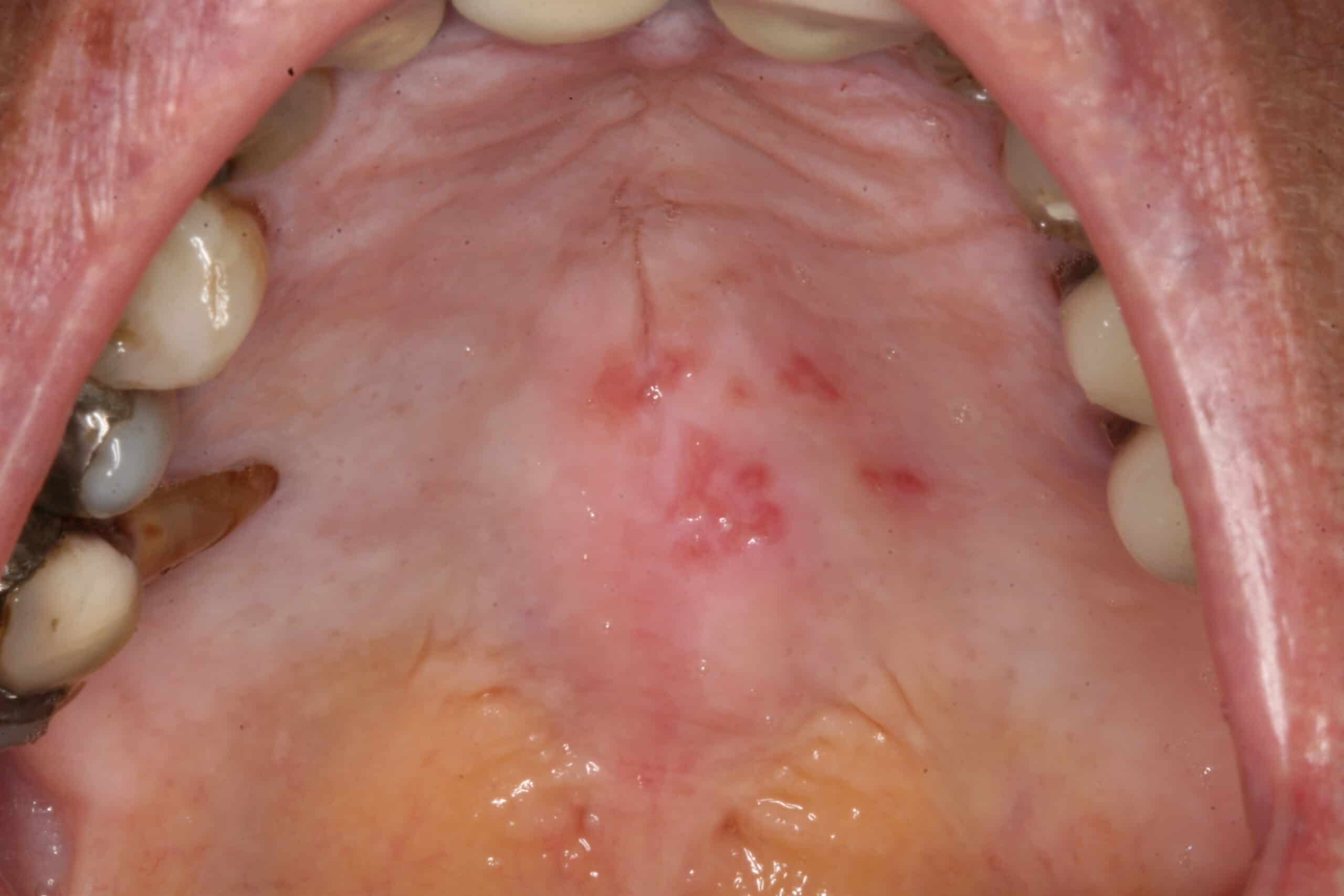 Herpes Simplex 1: Palate. Benign. Viral infection. Herpes can form inside the mouth on fixed tissue (tougher gum tissue) and is usually unilateral (not crossing the midline of the body).
Herpes Simplex 1: Palate. Benign. Viral infection. Herpes can form inside the mouth on fixed tissue (tougher gum tissue) and is usually unilateral (not crossing the midline of the body).
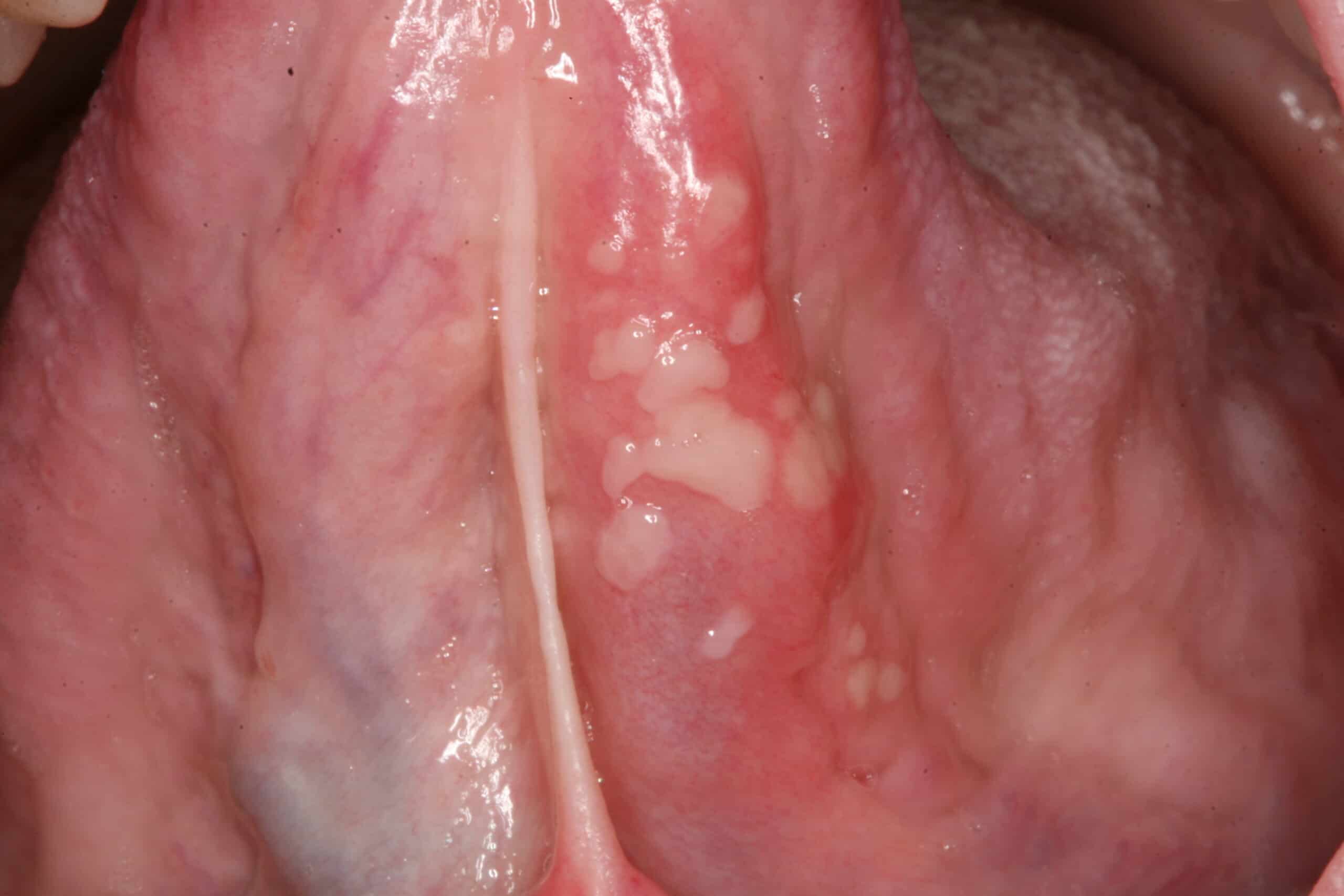 Unknown viral infection: Under tongue. Benign. Viral infection. There are many types of viruses that can infect the mouth.
Unknown viral infection: Under tongue. Benign. Viral infection. There are many types of viruses that can infect the mouth.
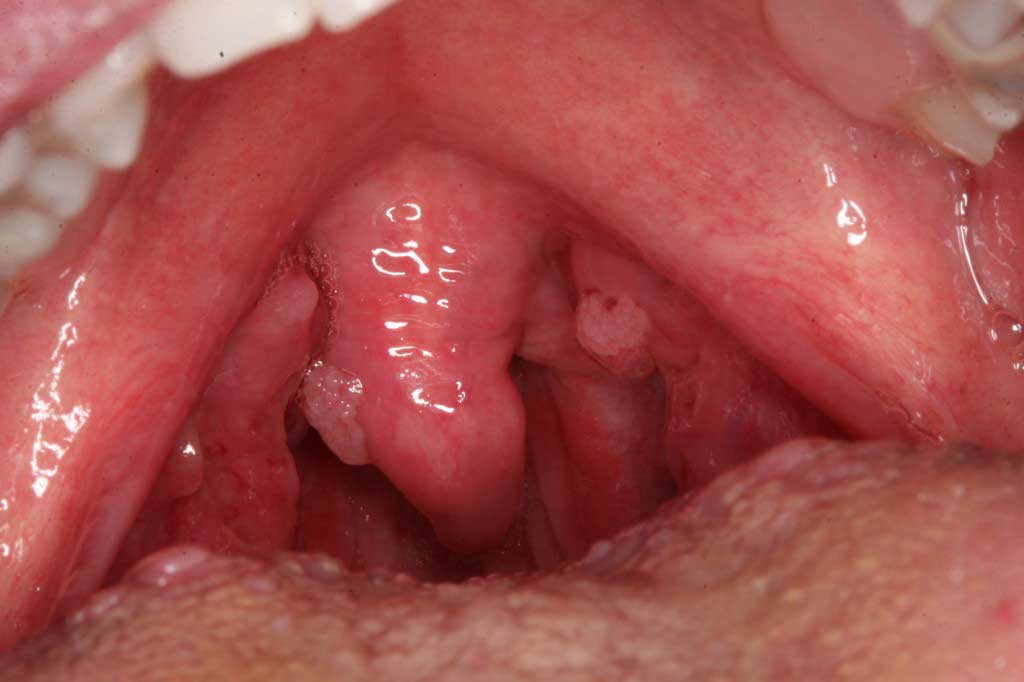
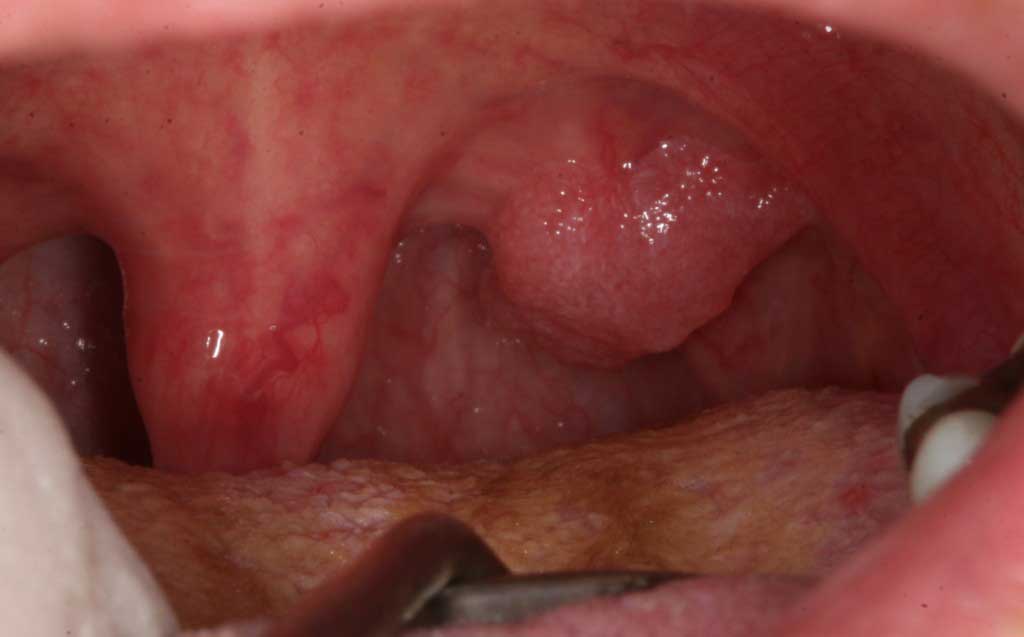
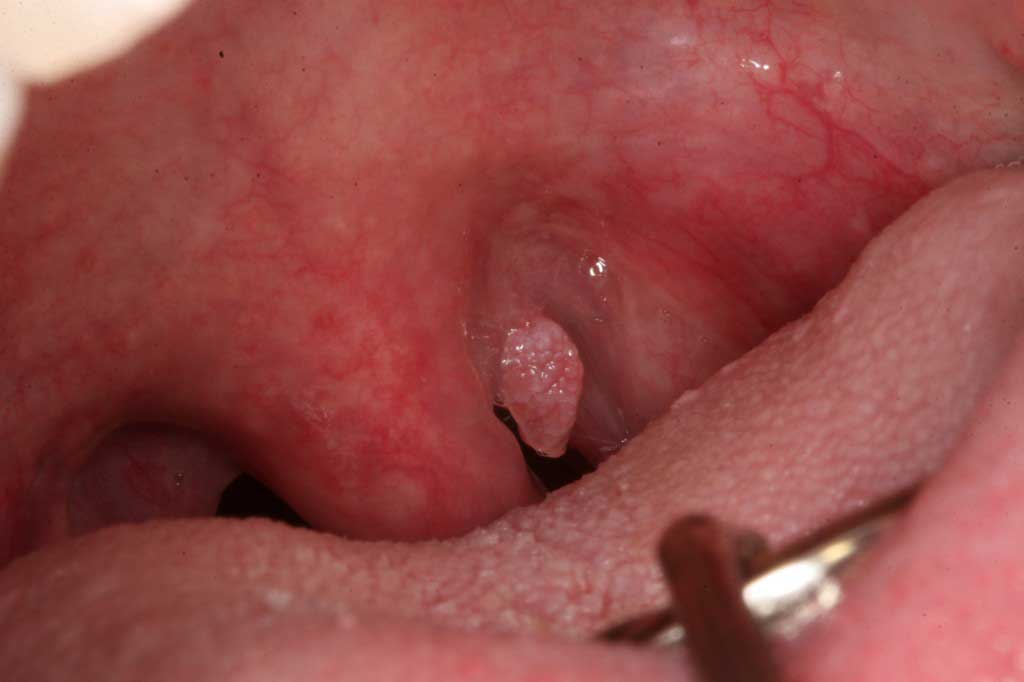 Human Papilloma Virus: Uvula. Venereal wart. A commonly found lesion in the mouth. (Pre-cancerous in combination with heavy smoking and alcohol usage)
Human Papilloma Virus: Uvula. Venereal wart. A commonly found lesion in the mouth. (Pre-cancerous in combination with heavy smoking and alcohol usage)
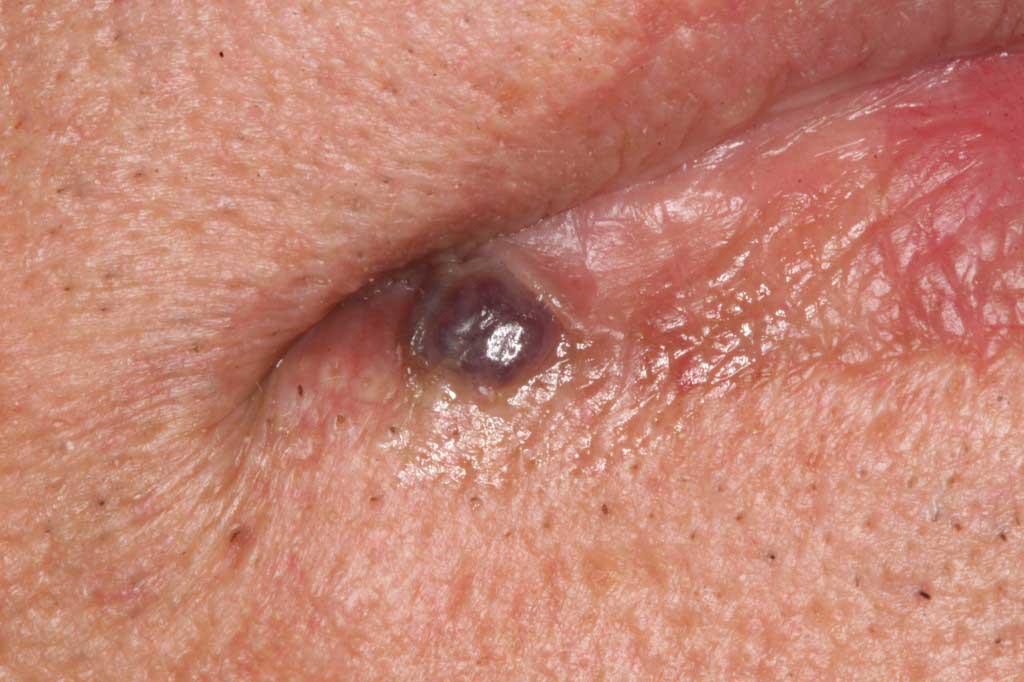
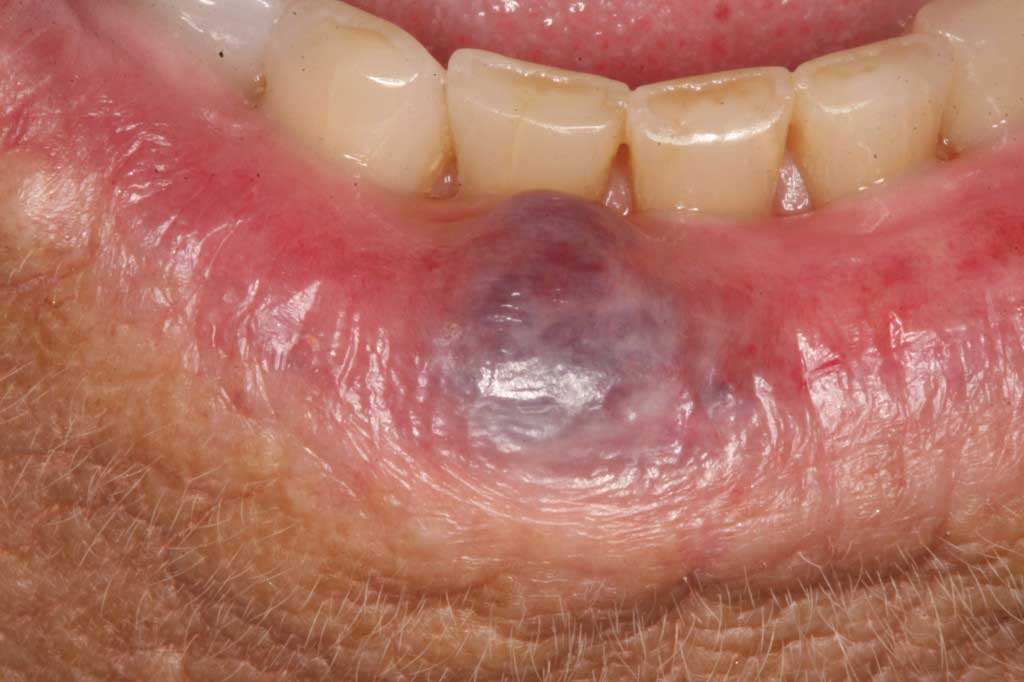
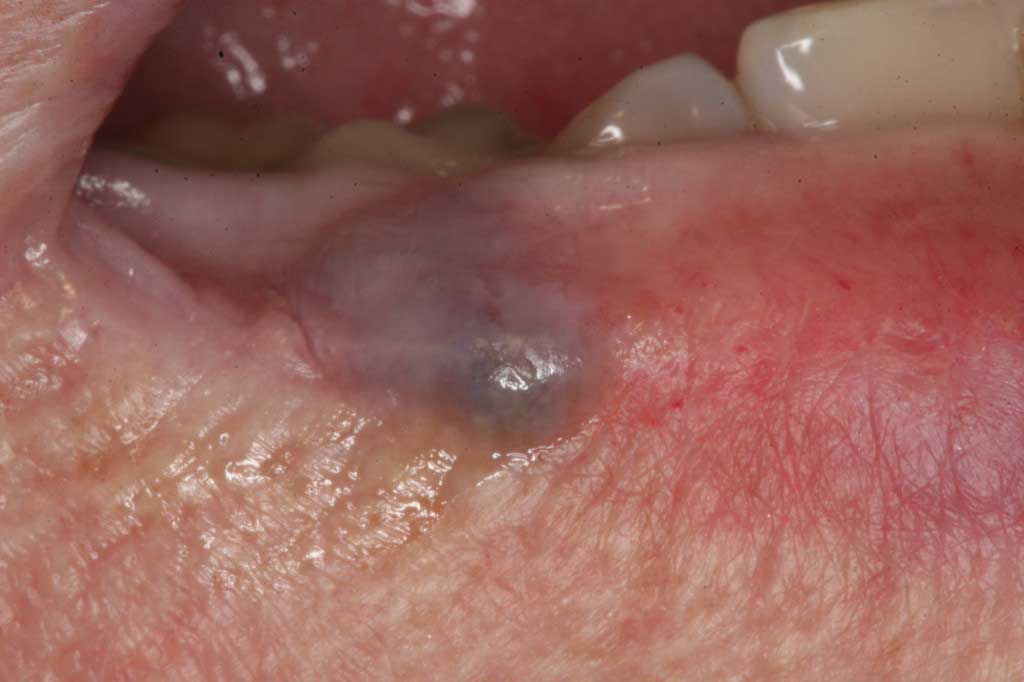
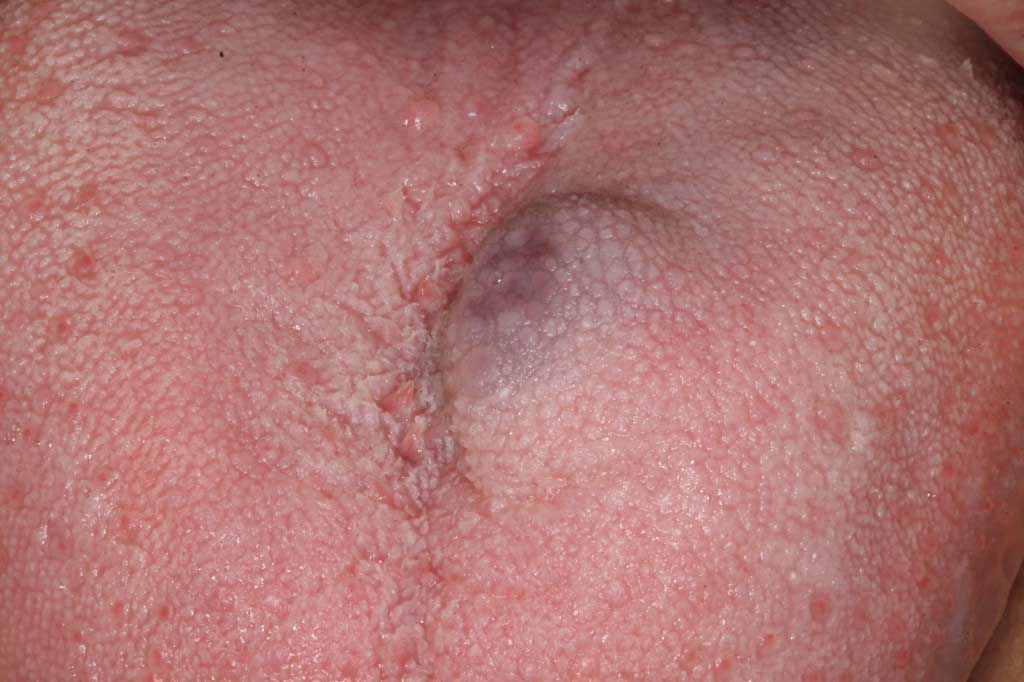 Hemangioma: Lower lips and tongue. Benign. Blood vessel filled lesion usually cause by trauma easily removed with a laser.
Hemangioma: Lower lips and tongue. Benign. Blood vessel filled lesion usually cause by trauma easily removed with a laser.
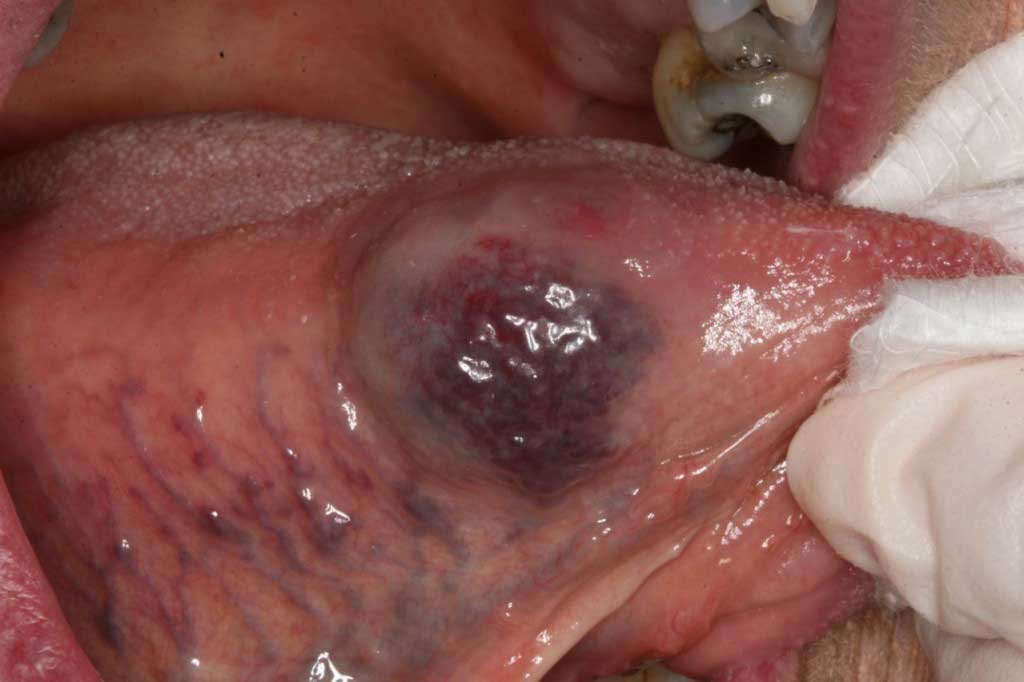
Hemangioma: Lateral border of tongue. The patient has had this on her tongue since birth.
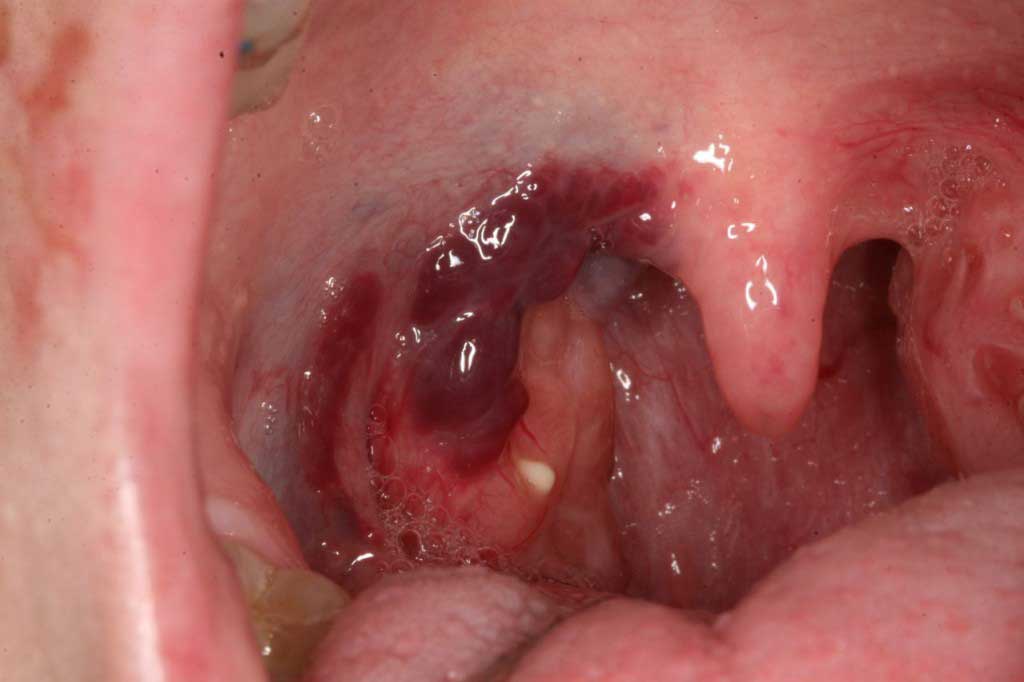
Tonsillar Hemangioma: Congenital blood vessel mass on right tonsillar pillar and soft palate that could become life threatening if it was traumatized and bleed enough to obstructed breathing.
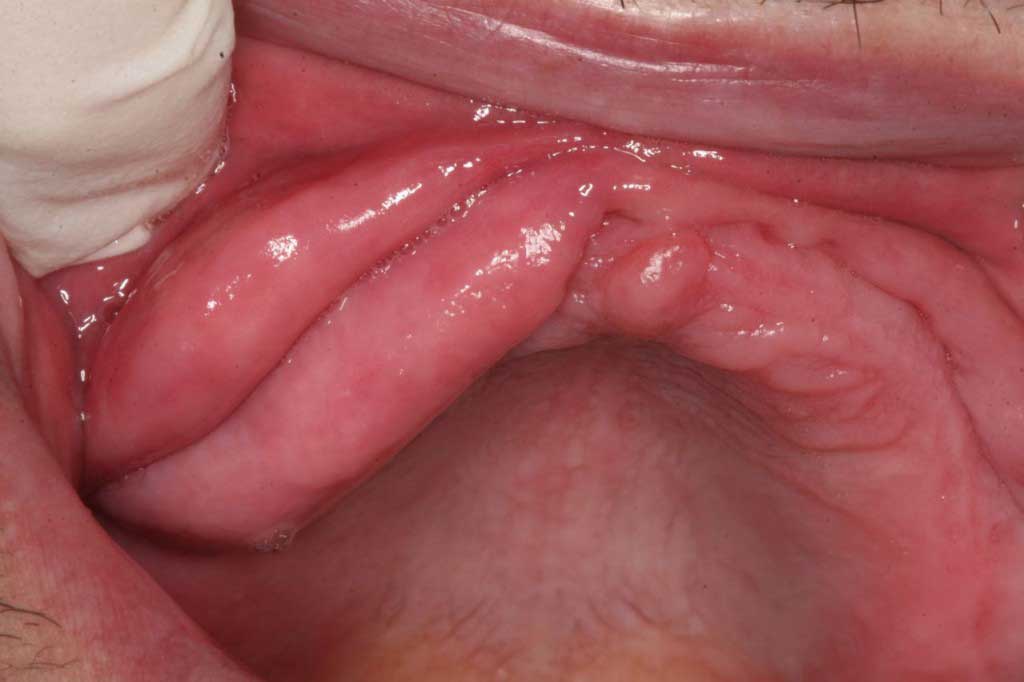
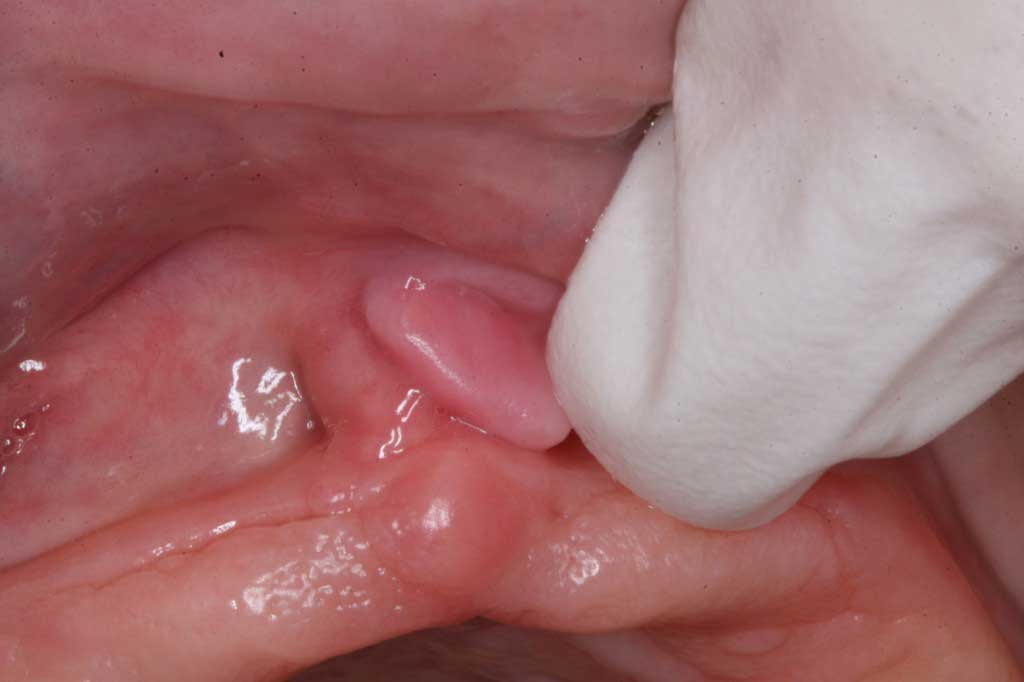 Epulis Fissuratum: Benign. Scarring from a denture sore under the upper lip. Treated by first removing the cause of the sore spot and letting the lesion shrink away, then relining the denture. If it does not go away, then the extra tissue is easily removed with a laser before relining the denture.
Epulis Fissuratum: Benign. Scarring from a denture sore under the upper lip. Treated by first removing the cause of the sore spot and letting the lesion shrink away, then relining the denture. If it does not go away, then the extra tissue is easily removed with a laser before relining the denture.
Epulis Fissuratum: This denture sore had not been addressed for many years. The tissue had piled up over top of the denture in two separate occasions to make this lesion look like lips inside his upper lip. It was removed with a laser and complete recovered with a relining of the upper complete denture.
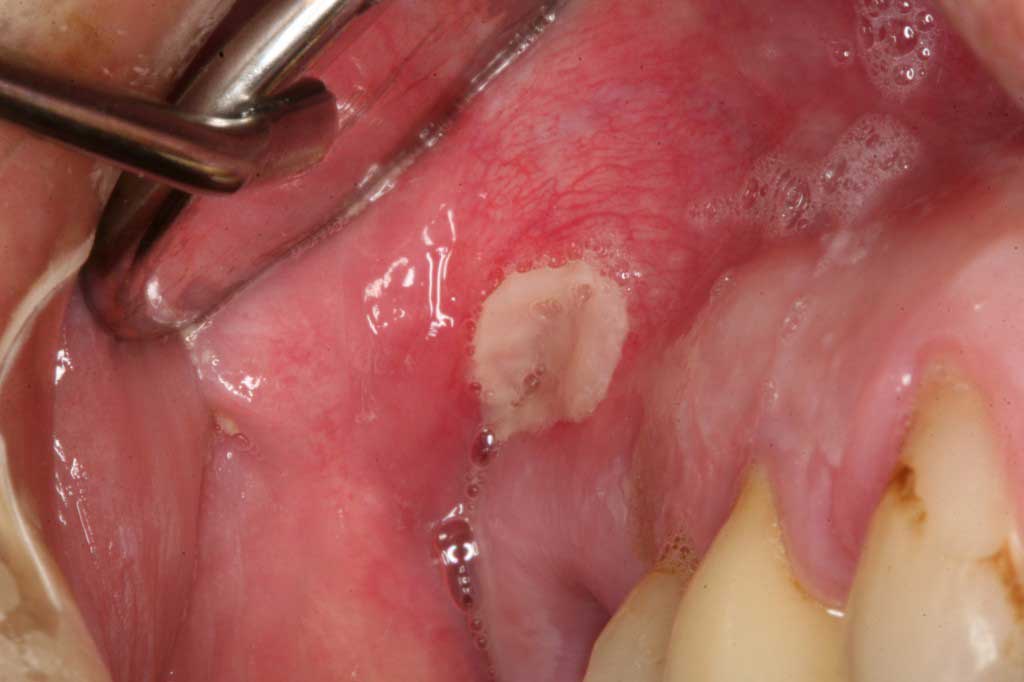 Denture sore: Back upper cheek. Benign. Ill-fitting denture can cut into the softer tissues causing a sore spot that is easily treated. Once the denture has been adjusted properly the lesion will go away.
Denture sore: Back upper cheek. Benign. Ill-fitting denture can cut into the softer tissues causing a sore spot that is easily treated. Once the denture has been adjusted properly the lesion will go away.
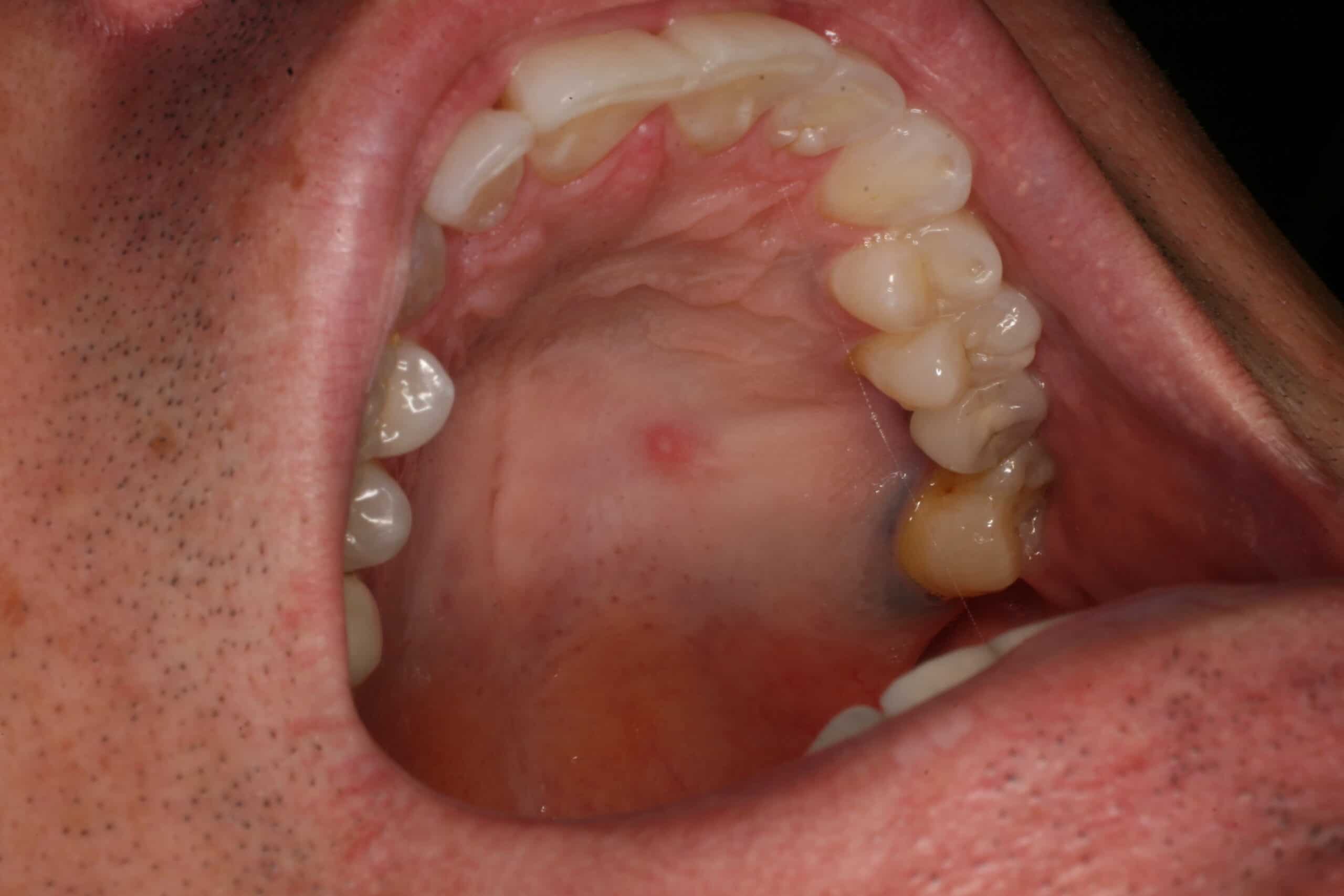 Mucocele: Benign. This is a damage minor salivary gland that backs up with saliva, and causes a little pimple. The lesion has been completely removed with a punch biopsy twice, and has returned each time. Notice the amalgam tattoo on the lingual of the second molar.
Mucocele: Benign. This is a damage minor salivary gland that backs up with saliva, and causes a little pimple. The lesion has been completely removed with a punch biopsy twice, and has returned each time. Notice the amalgam tattoo on the lingual of the second molar.
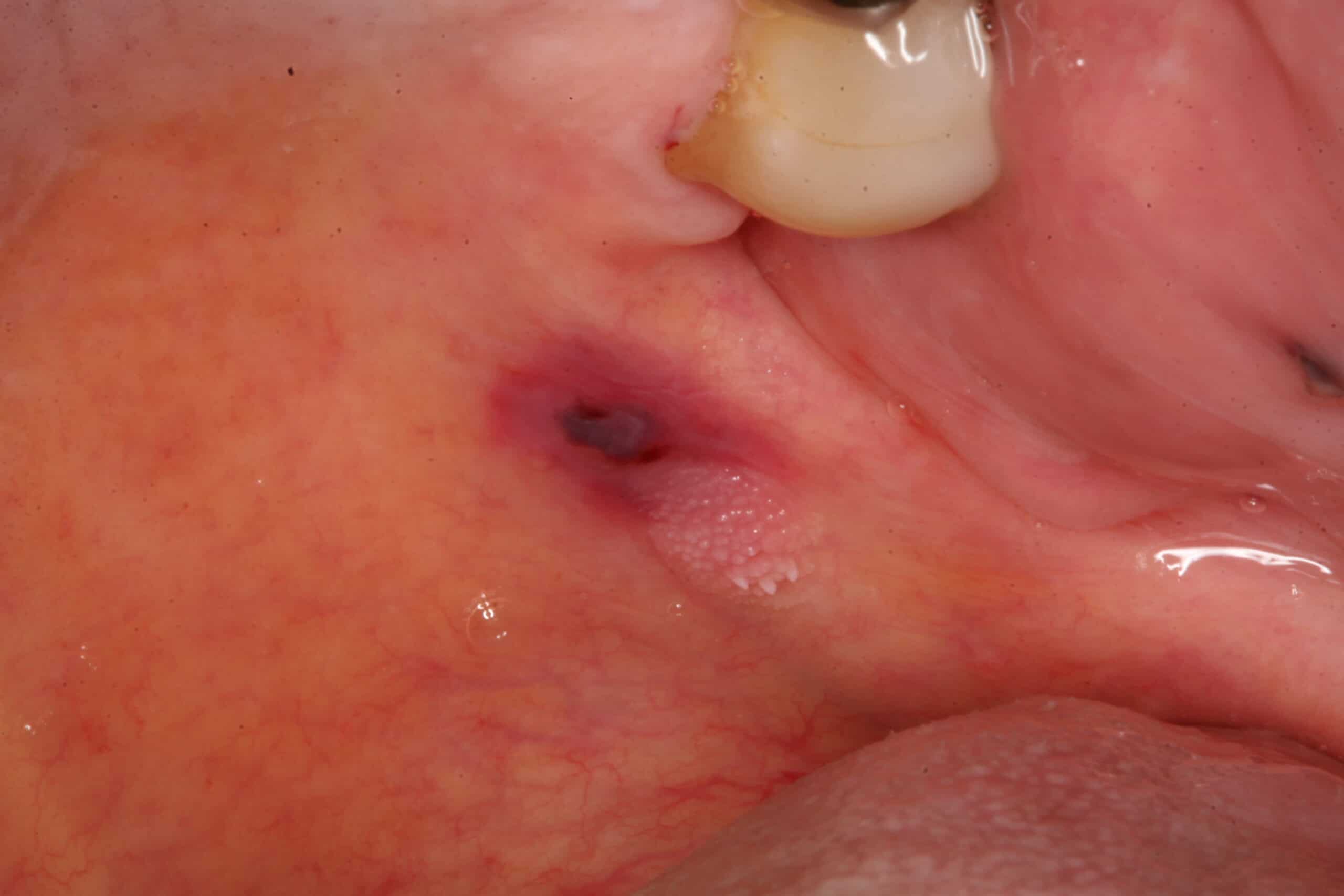 Trauma next to wart: Back upper palate. Sometime multiple lesions can present themselves next to each other. In this case food trauma (Dorito syndrome) is next to a venereal wart.
Trauma next to wart: Back upper palate. Sometime multiple lesions can present themselves next to each other. In this case food trauma (Dorito syndrome) is next to a venereal wart.
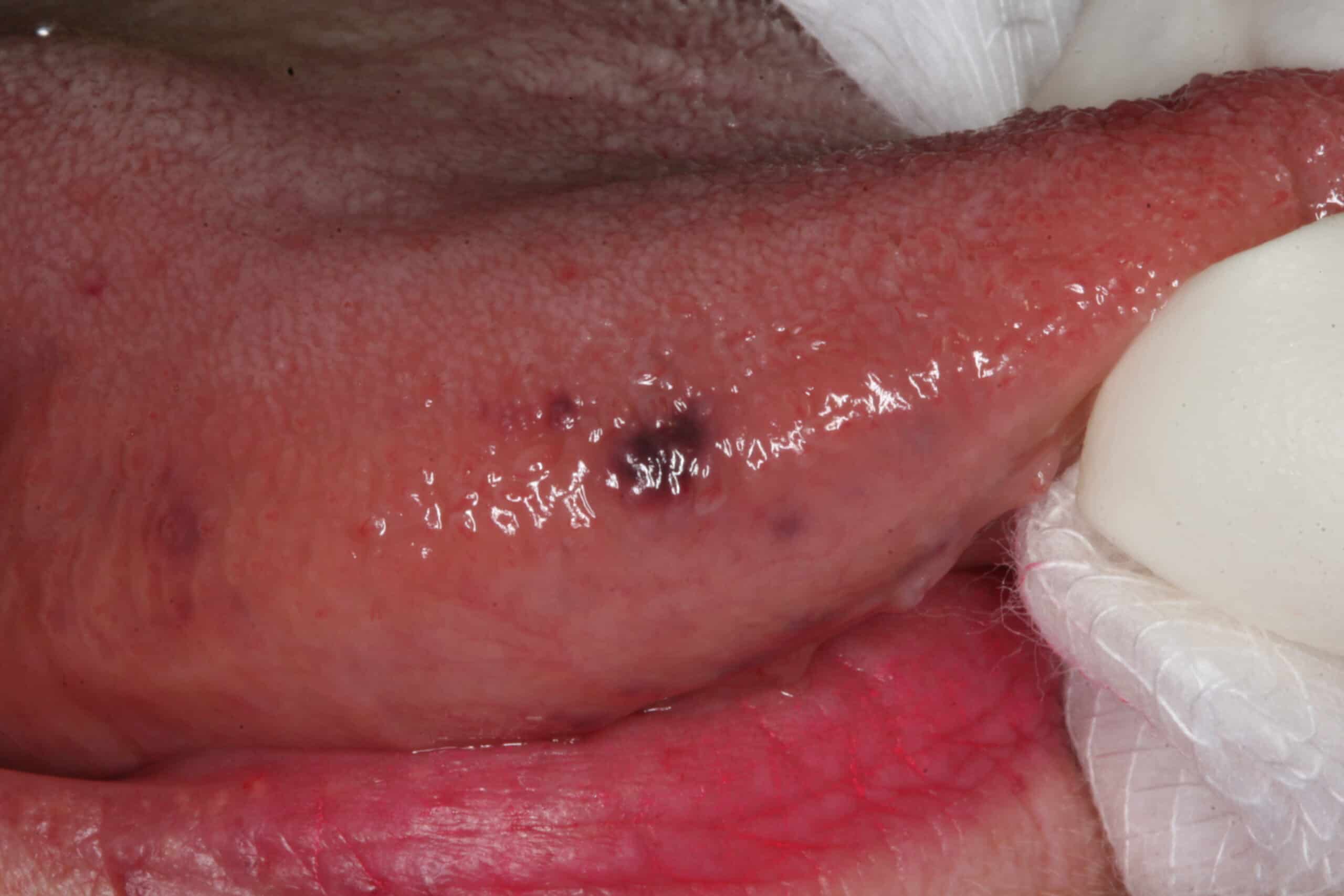 Tongue trauma: This lesion is from a bit tongue. However, it should be monitored for possible melanoma for a period of one month.
Tongue trauma: This lesion is from a bit tongue. However, it should be monitored for possible melanoma for a period of one month.
Lichen Planus: White streaked lesions form on cheeks and gums. Usually benign unless it becomes erosive.
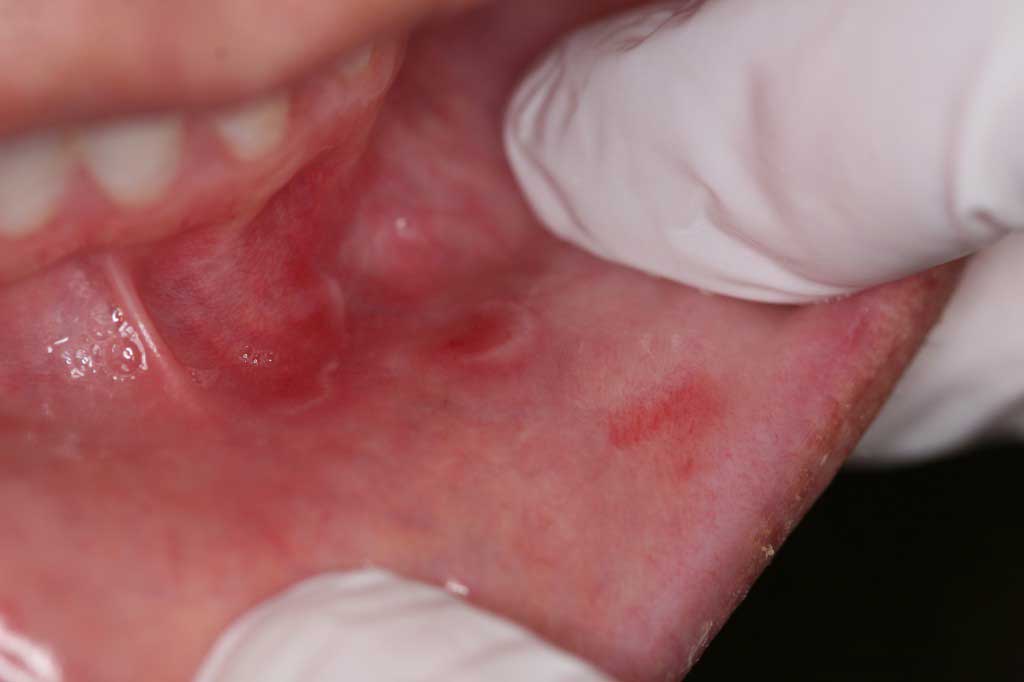 Benign Migratory Mucositis: Lower inside lip. This is more commonly seen on the tongue where it is called geographic tongue. This lesion was all over her tongue as well.
Benign Migratory Mucositis: Lower inside lip. This is more commonly seen on the tongue where it is called geographic tongue. This lesion was all over her tongue as well.
Geographic Tongue (Benign Migratory Glossitis): Benign, Unknown etiology
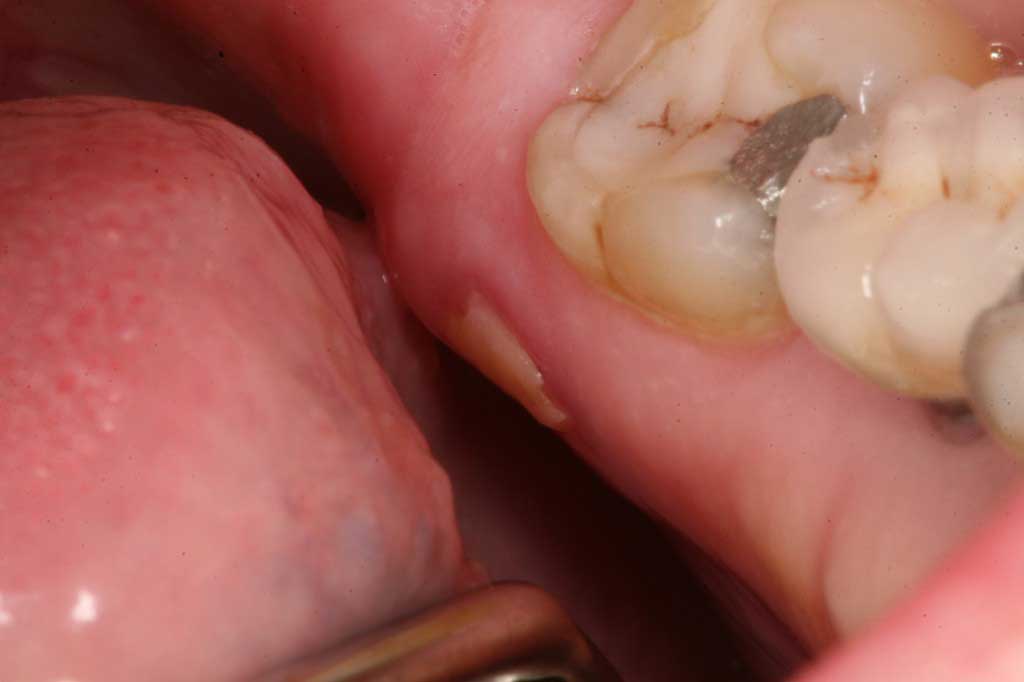 Bisphosphonate-assocoated Osteonecrosis: Lower molar. Cancer chemotherapy
Bisphosphonate-assocoated Osteonecrosis: Lower molar. Cancer chemotherapy
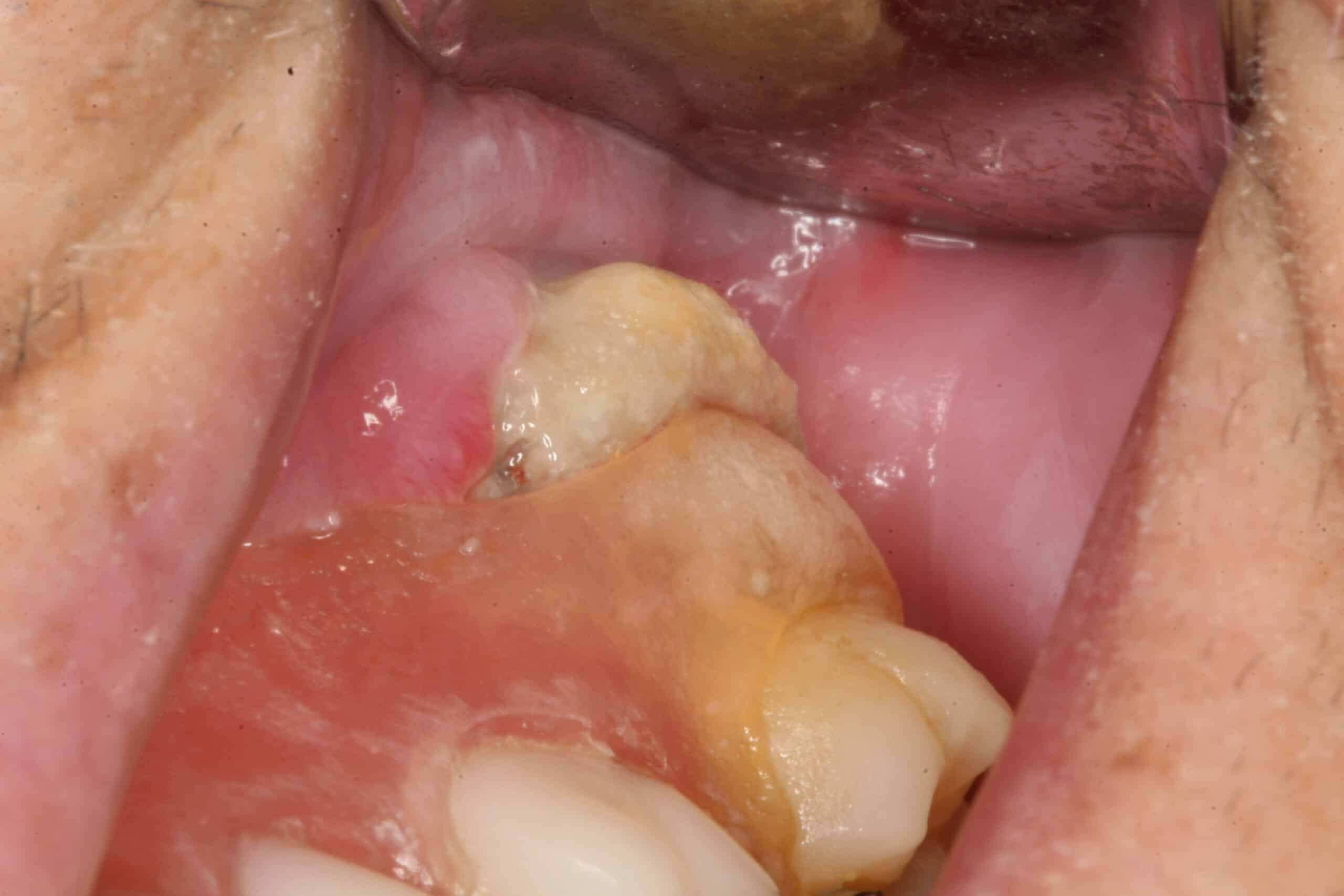
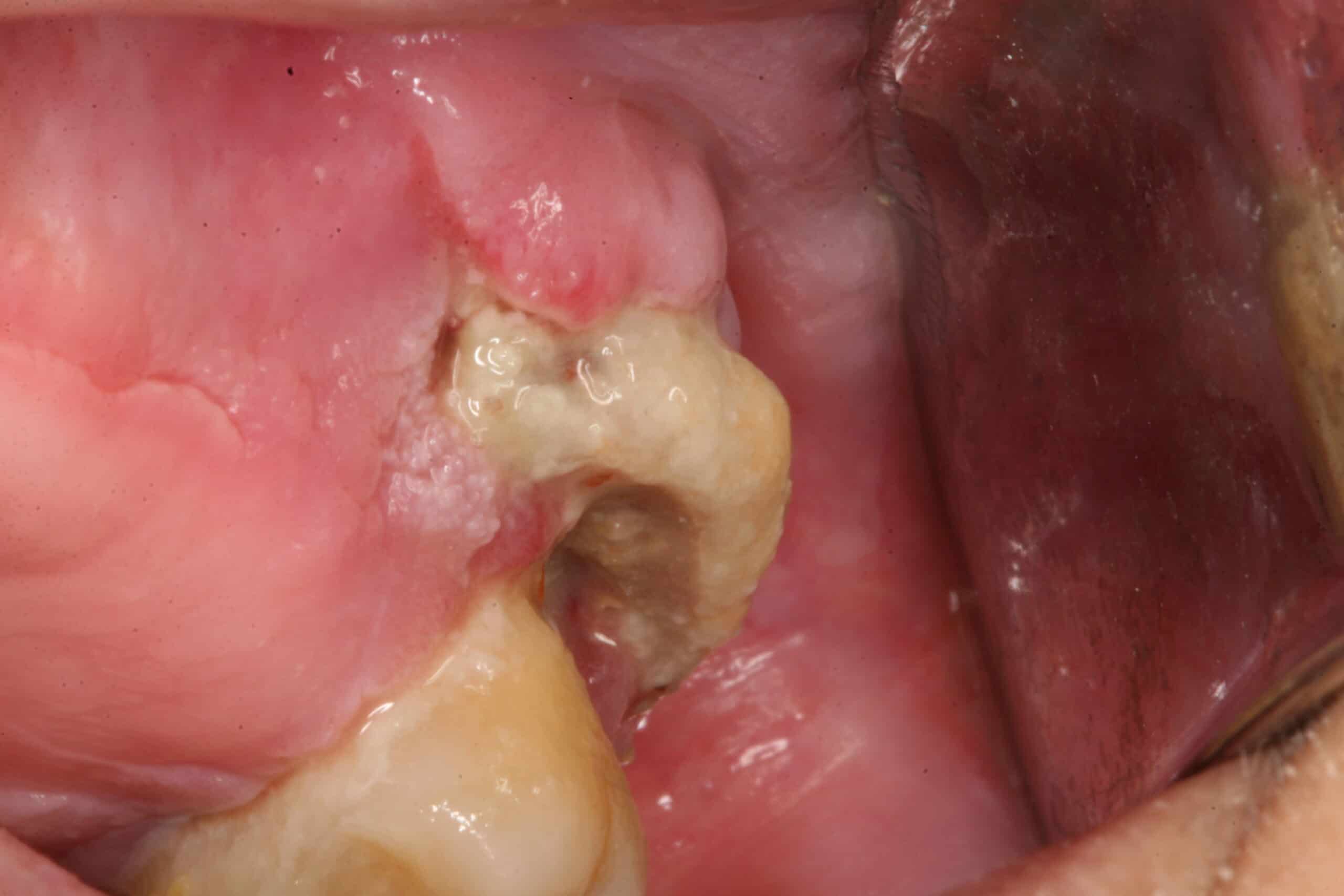
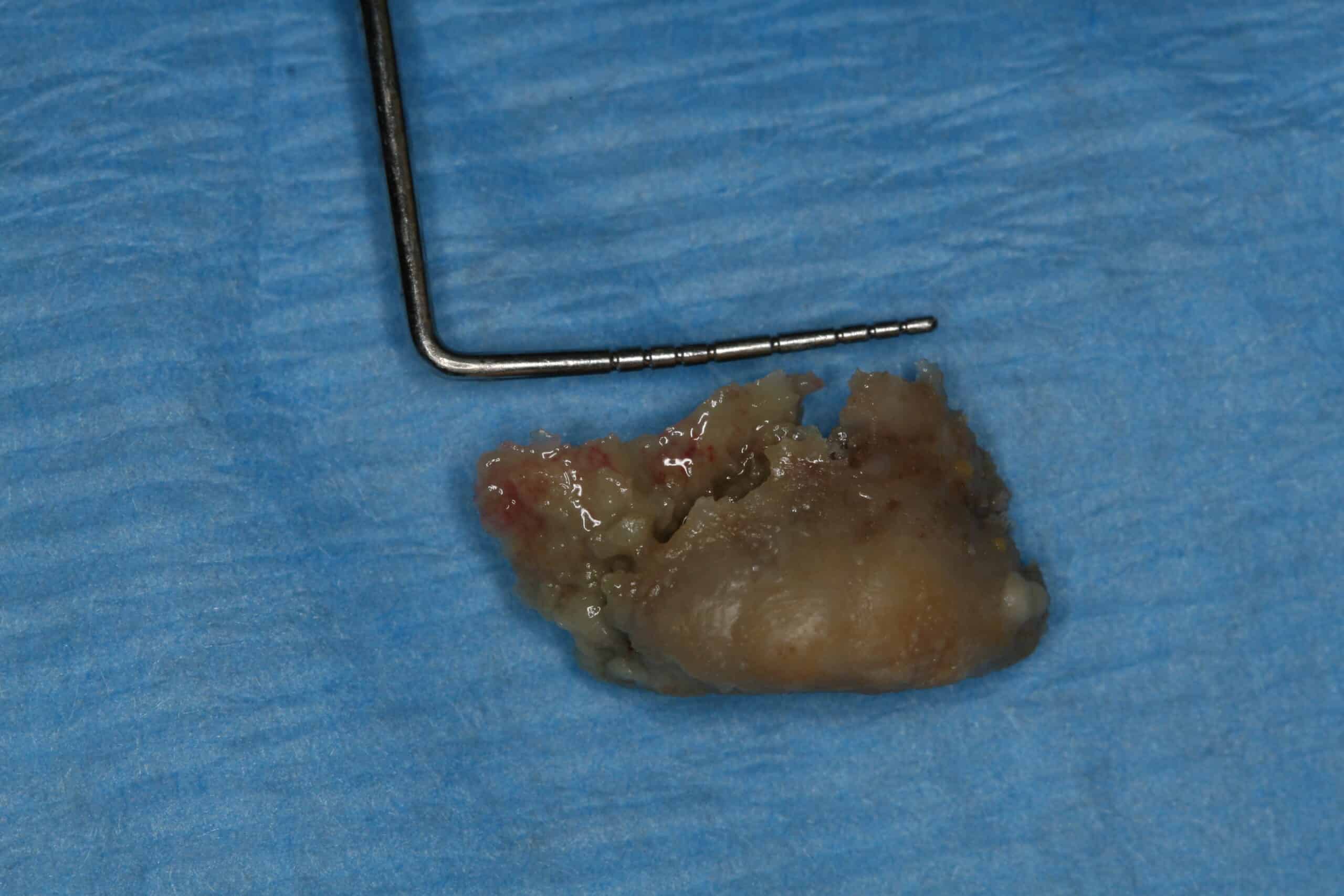
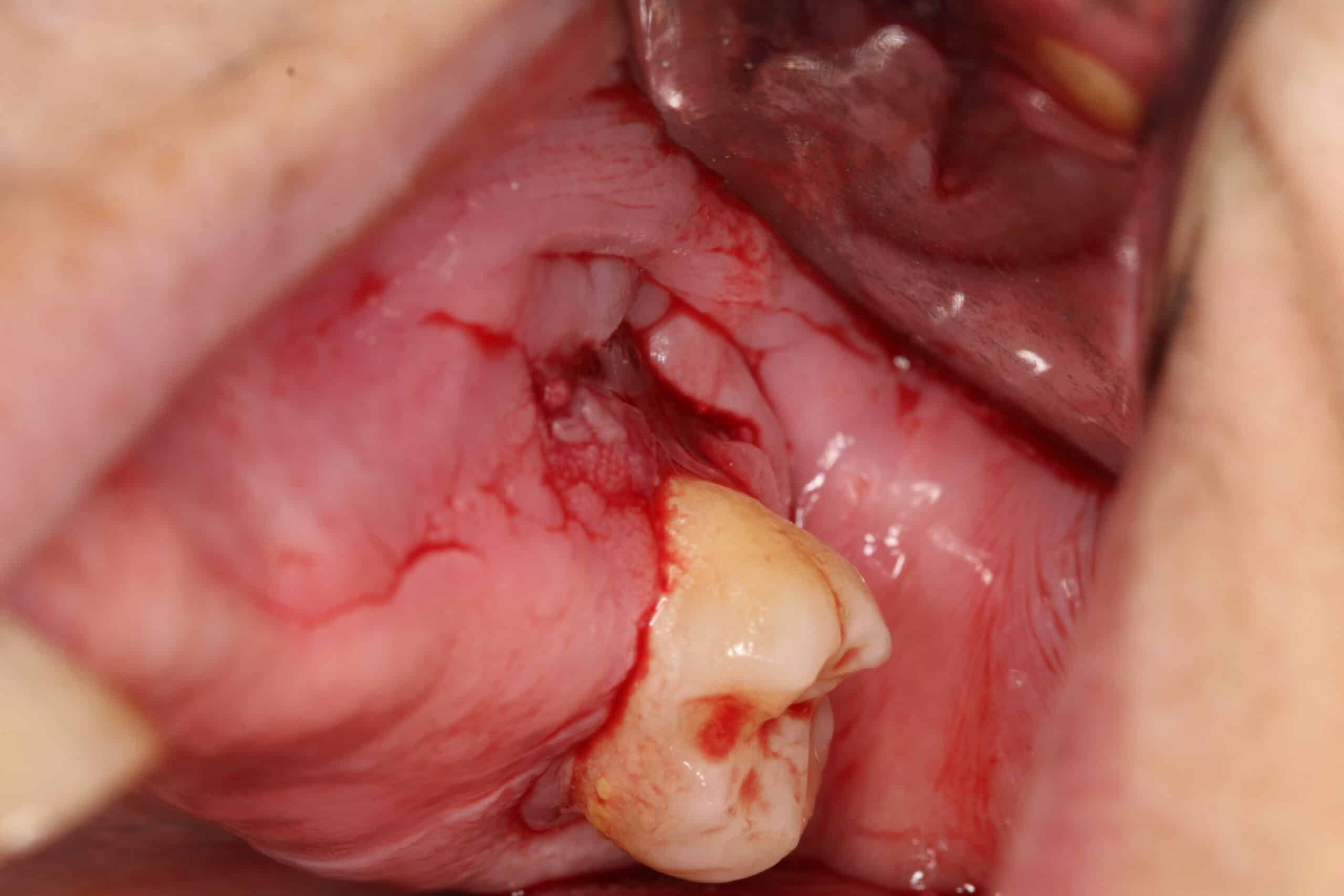 Bisphosphonate-associate Osteonecrosis: Upper molar. This patient had been on cancer chemotherapy and spontaneously developed this dead boney lesion under her partial denture. The lesion was self-limiting and healed after removing the dead bone.
Bisphosphonate-associate Osteonecrosis: Upper molar. This patient had been on cancer chemotherapy and spontaneously developed this dead boney lesion under her partial denture. The lesion was self-limiting and healed after removing the dead bone.
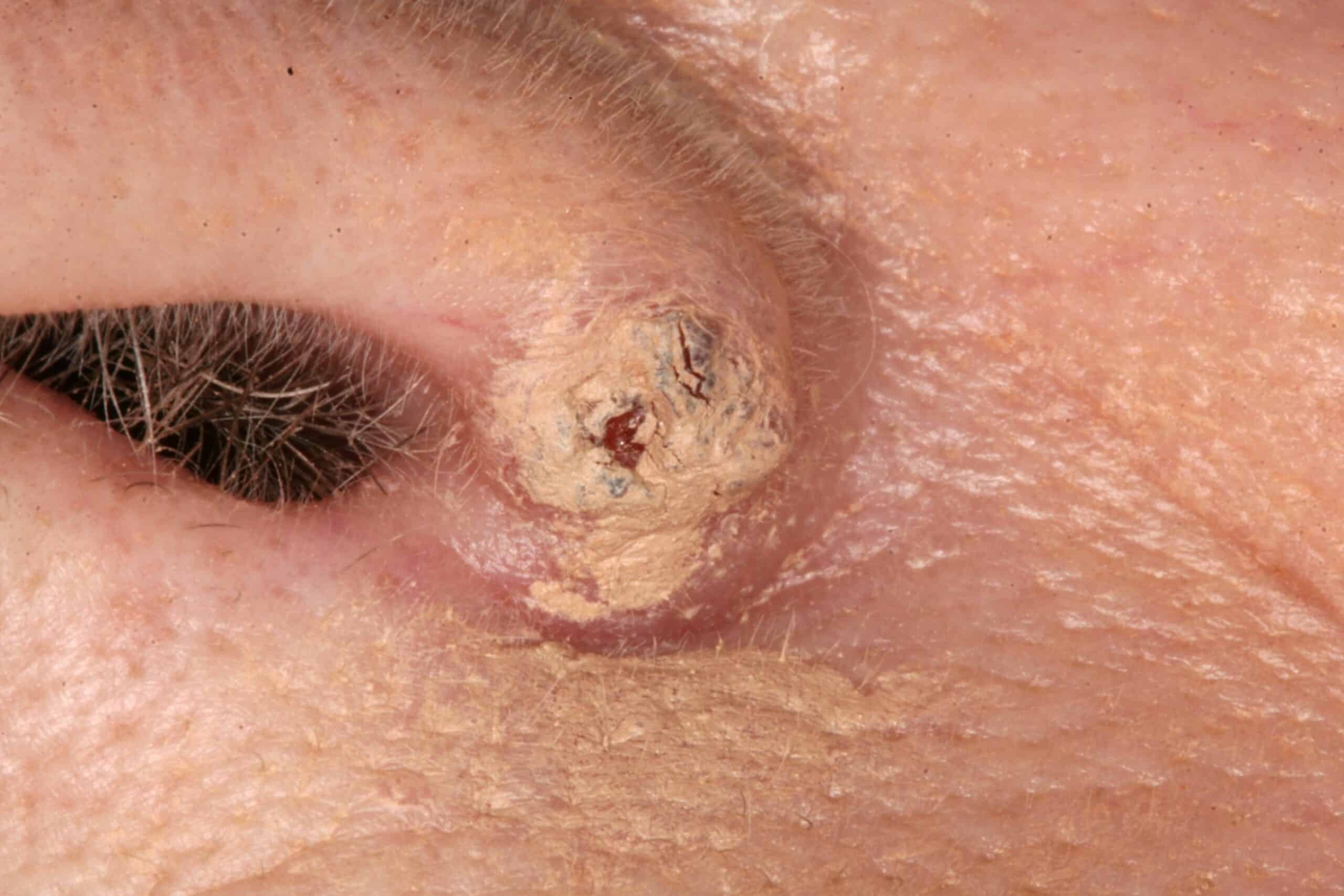
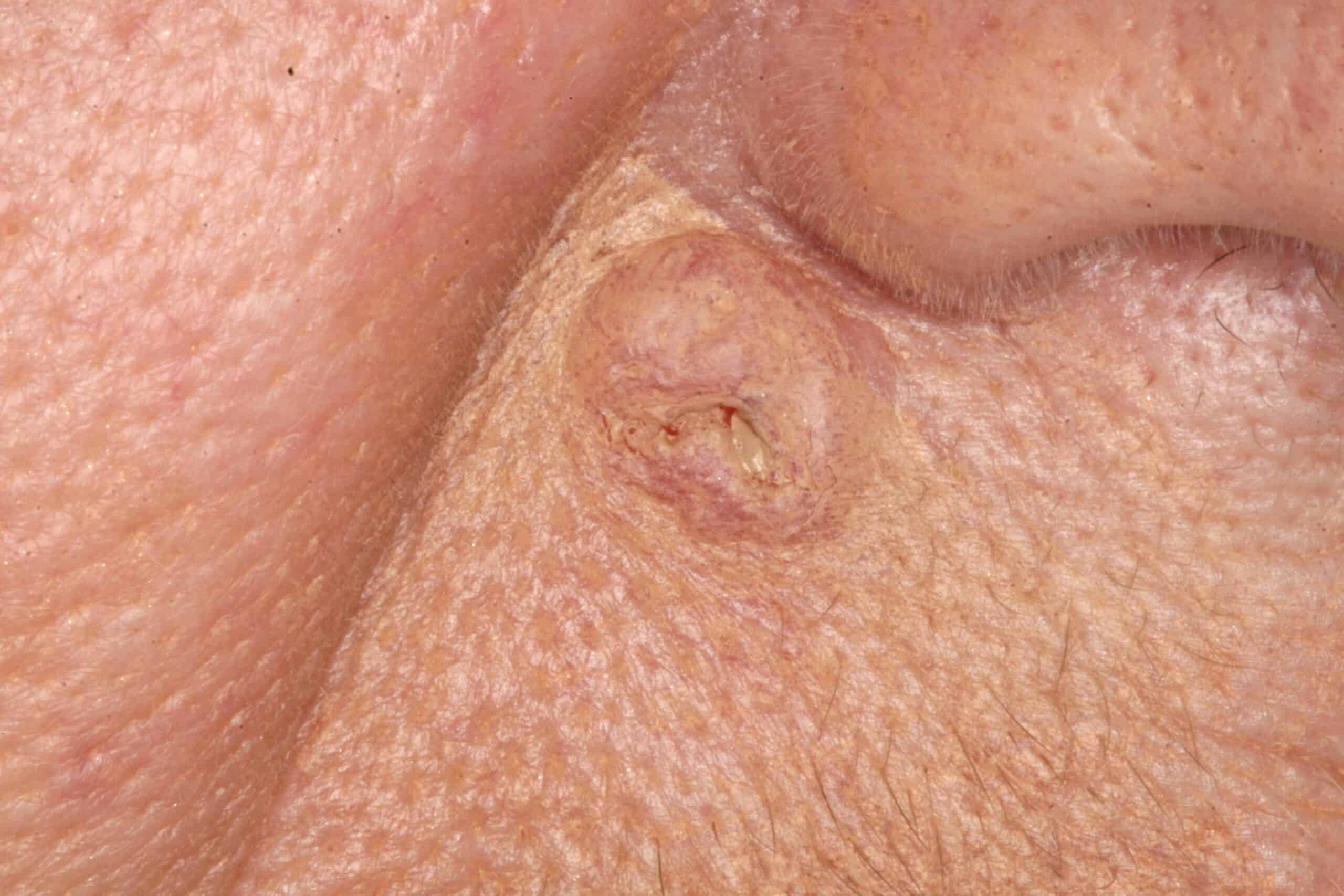 Basal cell carcinoma: Cancer. This lady thought if she just covered it with make-up it would go away.
Basal cell carcinoma: Cancer. This lady thought if she just covered it with make-up it would go away.
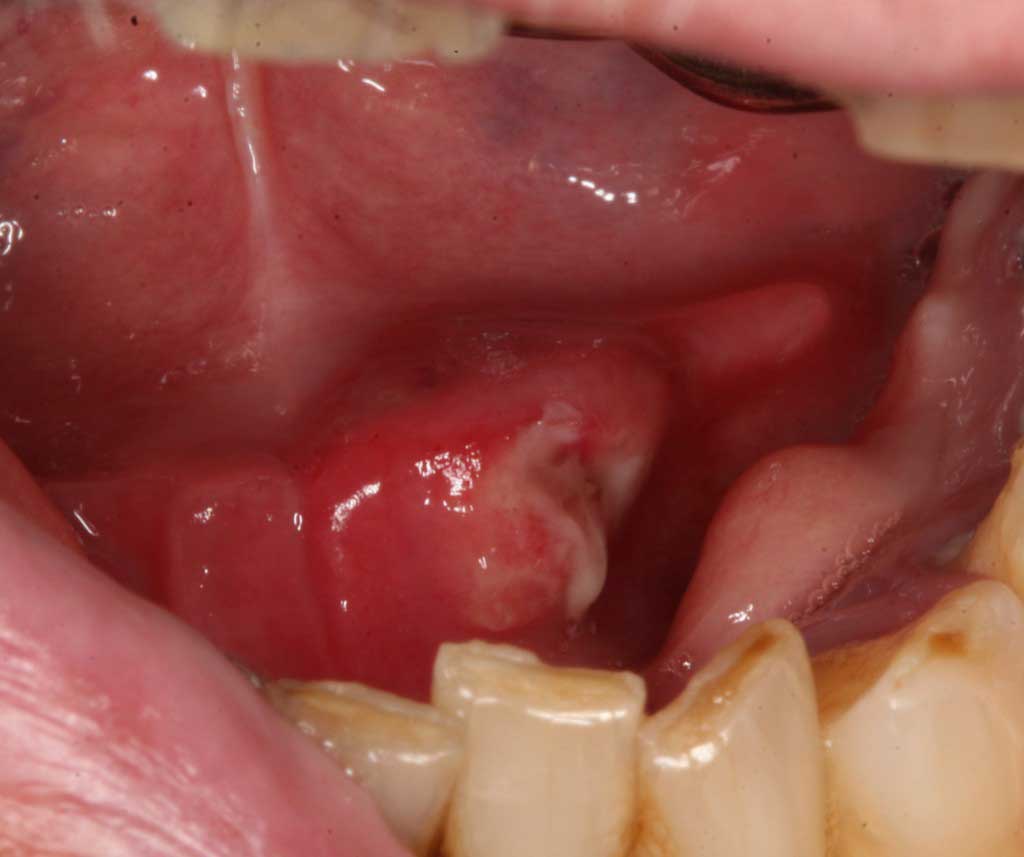 Squameous cell carcinoma: Cancer. Malignant. Under the tongue is a high risk area for carcinomas.
Squameous cell carcinoma: Cancer. Malignant. Under the tongue is a high risk area for carcinomas.
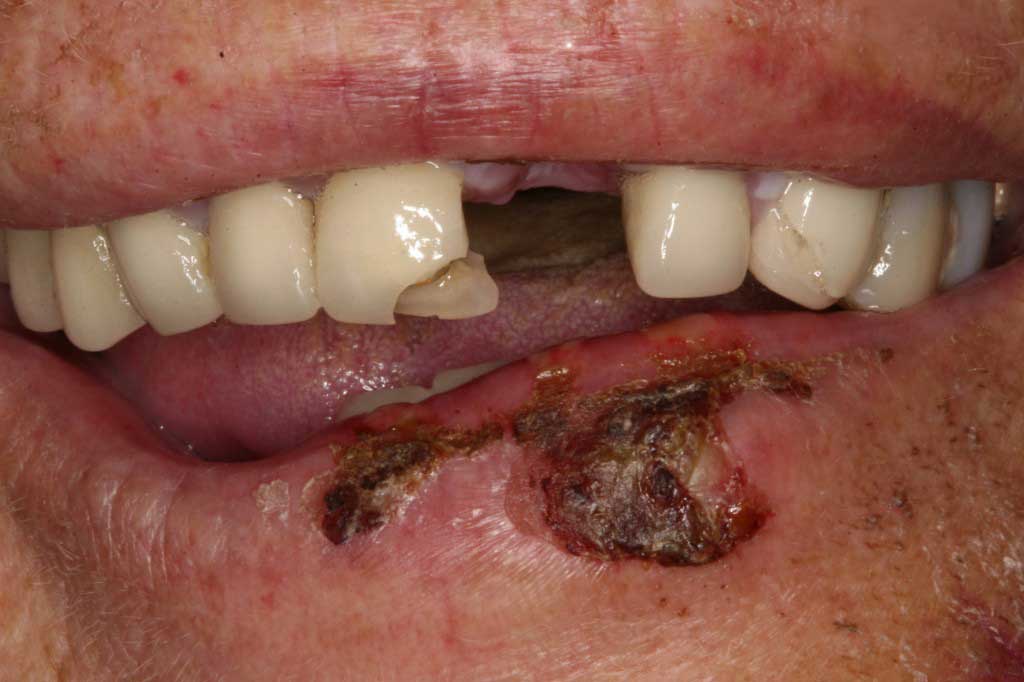
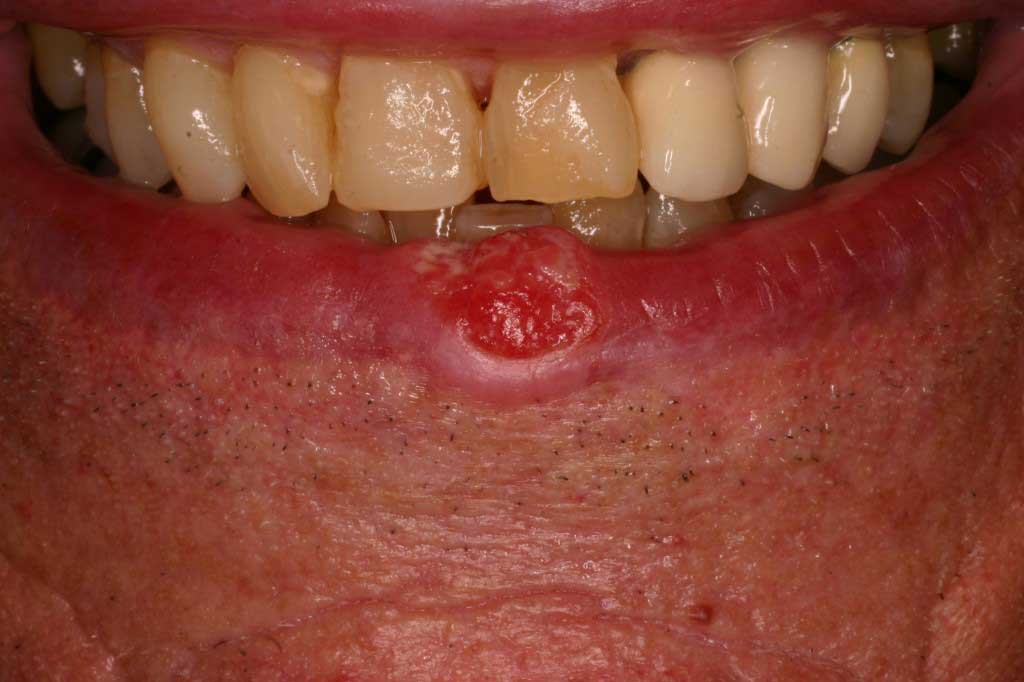 Squameous cell carcinoma: Cancer. Malignant. Years of sun damage. Rule-of-thumb: If you have a red and/or crusty lesion on your lip that lasts more than 2 weeks, then it is at high risk of being cancer.
Squameous cell carcinoma: Cancer. Malignant. Years of sun damage. Rule-of-thumb: If you have a red and/or crusty lesion on your lip that lasts more than 2 weeks, then it is at high risk of being cancer.
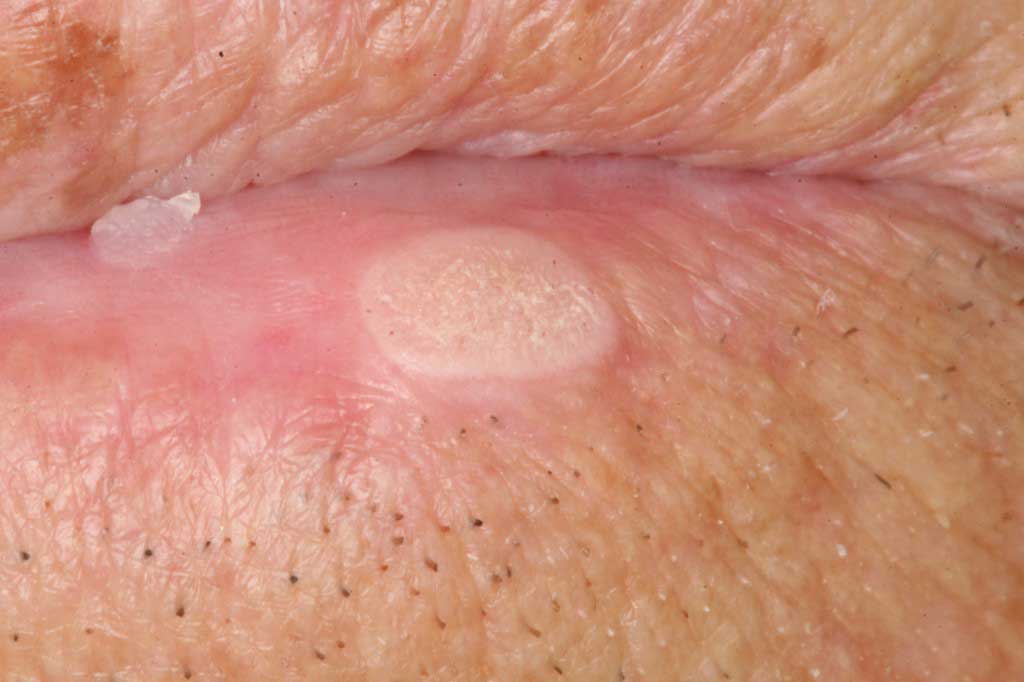
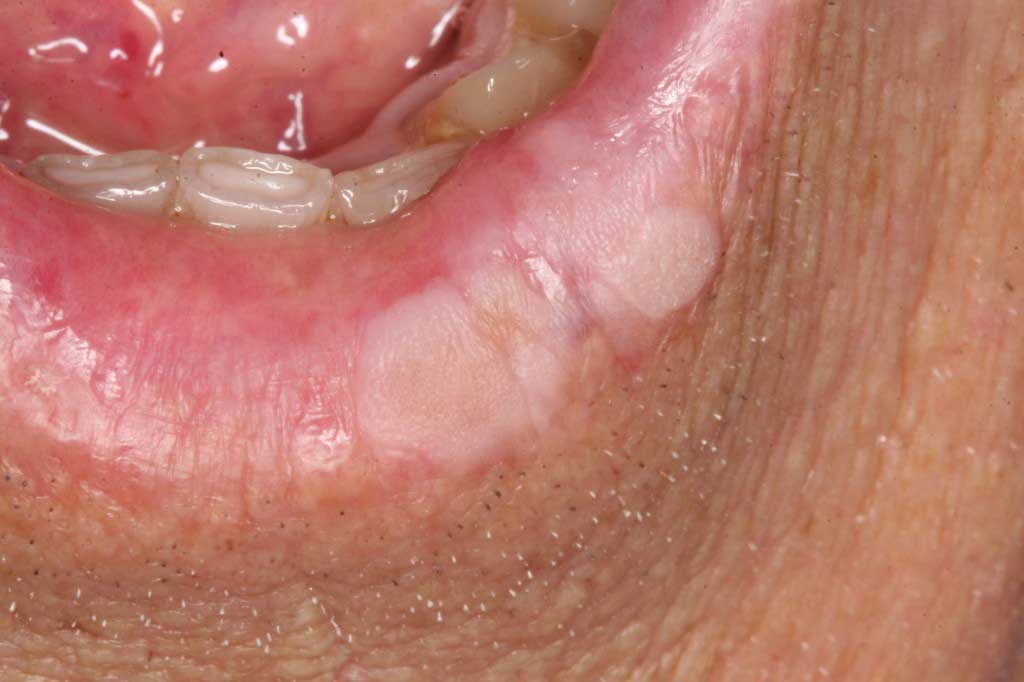 Seborrheic Keritosis: Benign wart-like skin tumor of unknown etiology.
Seborrheic Keritosis: Benign wart-like skin tumor of unknown etiology.
Psoriasis of the Tongue: Benign. The differential diagnosis included Lichen Planus, Benign Migratory Mucositis (Geographic Tongue), trauma, Squamous Cell Carcinoma. This was diagnosed with a biopsy.
Aphthous Ulcer: Benign. These lesions are very common and can be diagnosed over the phone (just kidding) by asking the patient if it burns when they place their tongue on it. Below and to the left is a benign traumatic “blood blister.”
Chemical Burn: Aspirin. This is an old “wives tale” placing aspirin over a toothache and is practiced all the time. The way this really works is the patient places an aspirin over the toothache and it dissolves in the mouth. The patient then swallows the aspirin and goes into the stomach where it is absorbed into the bloodstream. The aspirin then helps with pain control. Since aspirin is acetylsalicylic acid it causes a huge chemical burn where it is allowed to dissolve in the mouth. It would have been more effective if the patient simply swallowed the aspirin in the first place.
Mucocele: Benign: Trauma. This is a backed-up minor salivary gland that’s opening was traumatized by either temperature burn, chemical burn or physical trauma. The treatment is draining. It has a high reoccurrence rate and if it reoccurs it is usually enucleated. This mucocele was caused by a volleyball to the face.
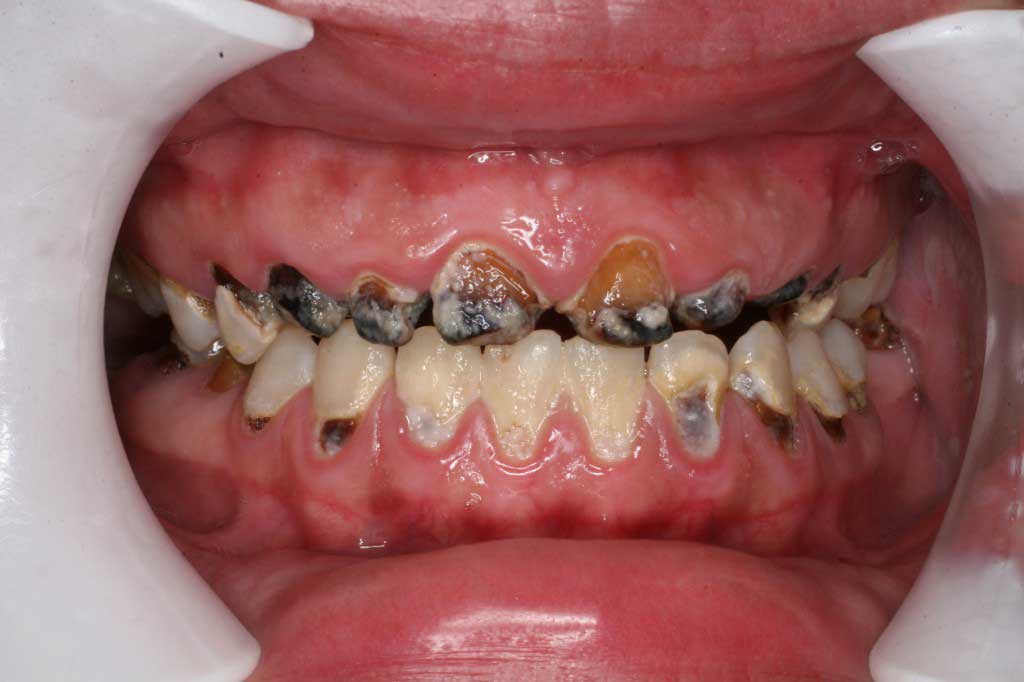
Radiation Caries: This is decay that was caused by a lack of salivary flow and ineffective oral hygiene. The patient had head and neck radiation for cancer and this destroyed their salivary glands. To have hopeless/painful teeth extracted, the patient will have to have hyperbaric oxygen treatments first to prepare the bone so osteoradionecrosis does not form in the healing site(s).
Traumatic “Blood Blister”: Benign. Caused by trauma to the oral mucosa such as biting the cheek and is usually slightly raised. If you “pop it” with an explorer a small amount of old blood will appear and the lesion will quickly heal.
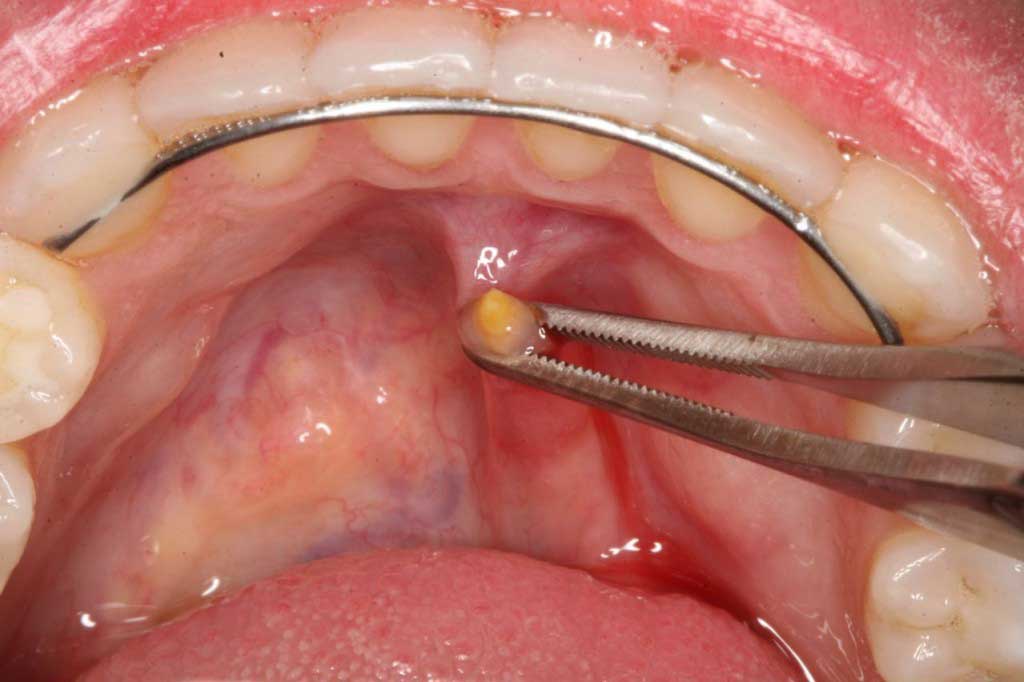
Sialolith: Submandibular duct stone. She went to her MD and told him it swelled under her jaw when she ate food. He told her it was just an ulcer and gave her some antibiotics. The stone was teased out and she felt much better immediately when a copious amount of saliva shot out of the duct upon the stones removal from the back pressure created by the blocked duct..
More lesion photos to come…
References:
1. Rev Assoc Med Bras. 2011 Apr;57(2):171-176. Tobacco and alcohol use after head and neck cancer treatment: influence of the type of oncological treatment employed.
[Article in English, Portuguese]Pinto FR, Matos LL, Gumz Segundo W, Vanni CM, Rosa DS, Kanda JL. Instituto do Câncer do Estado de São Paulo.
2. Br J Cancer. 2008 May 20;98(10):1653-61. Epub 2008 May 13. Cigarette smoke induces genetic instability in airway epithelial cells by suppressing FANCD2 expression. Hays LE, Zodrow DM, Yates JE, Deffebach ME, Jacoby DB, Olson SB, Pankow JF, Bagby GC. OHSU Cancer Institute, Oregon Health & Science University, 3181 Southwest Sam Jackson Park Road, Portland, OR 97239, USA. haysl@ohsu.edu
3. Oral Oncology Volume 37, Issue 8 , Pages 613-619, December 2001. Periodontal disease and periodontal management in patients with cancer. J.B. Epstein![]() , P. Stevenson-Moore
, P. Stevenson-Moore
4. Nutr Cancer. 2011 May 2:1-11. Weight Change and Its Correlates Among Breast Cancer Survivors. Chen X, Lu W, Gu K, Chen Z, Zheng Y, Zheng W, Shu XO. Department of Medicine, Vanderbilt Epidemiology Center, Vanderbilt University Medical Center and Vanderbilt-Ingram Cancer Center, Nashville, Tennessee, USA.
5. Fogorv Sz. 2009 Jun;102(3):103-9. [The oral lichen planus: doubts and evidence]. [Article in Hungarian] Tar I, Márton I. Debreceni Egyetem OEC, Fogorvostudományi Kar, Parodontológiai Tanszék, Restauratív Fogászati Tanszék, Debrecen.
6. Pediatr Nurs. 2011 May-Jun;37(3):115-8; quiz 119. Case study: Aphthous ulcers in a 14-year-old girl. Krebs KT. Primary Care Clinic, Child Health Associates, Warrenton, VA, USA.
7. Laryngorhinootologie. 2009 Feb;88(2):112-5. Epub 2008 Dec 8. [Metastatic Crohn’s disease: manifestation in head and neck region]. [Article in German] Hindersin S, Mönnighoff I, Schipper J, Hoffmann TK. Klinik für Hals-Nasen-Ohrenheilkunde, Universitätsklinikum Düsseldorf. simone.hindersin@uni-duesseldorf.de
8. Arch Pathol Lab Med. 2009 May;133(5):692-8. Necrotizing sialometaplasia: a practical approach to the diagnosis. Carlson DL. Department of Pathology, Memorial Sloan-Kettering Cancer Center, New York, New York 10065, USA. carlsond@mskcc.org9.
10. J Cancer Res Ther. 2012 Jan;8 Suppl:S111-5. Minor salivary gland tumors of the oral cavity: A case series with review of literature. Vaidya AD, Pantvaidya GH, Metgudmath R, Kane SV, D’Cruz AK. Department of Head and Neck Surgery, Tata Memorial Hospital, Mumbai, India.11. Pediatr Radiol. 2011 Oct 28. [Epub ahead of print] NUT midline carcinoma: an imaging case series and review of literature. Polsani A, Braithwaite KA, Alazraki AL, Abramowsky C, Shehata BM. Department of Radiology & Imaging Sciences, Children’s Healthcare of Atlanta, Emory University, 1405 Clifton Road NE, Atlanta, GA, 30322, USA, aruna_polsani@yahoo.com.